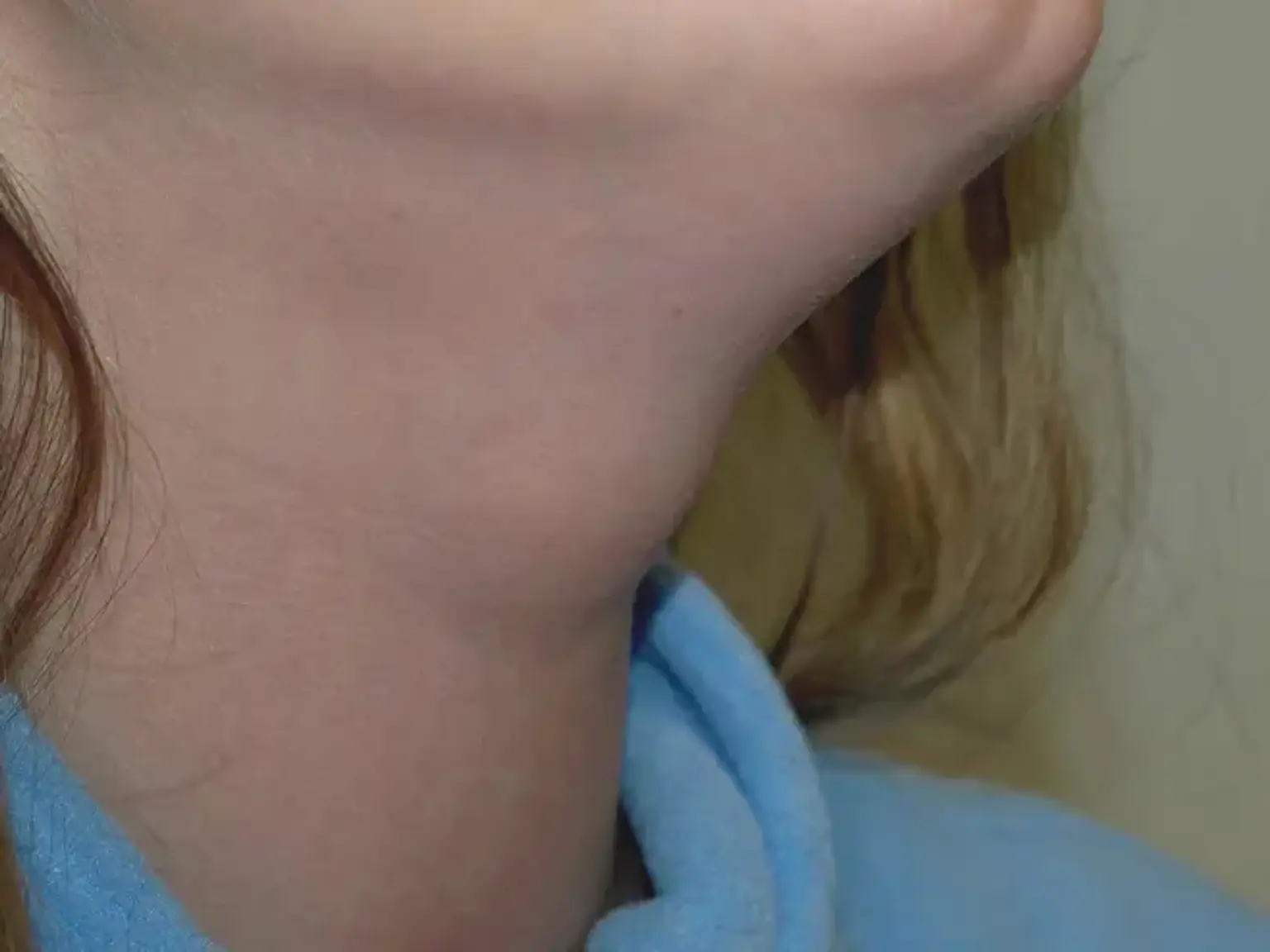
Thyroglossal duct cyst
Overview
The most frequent cervical anomaly is thyroglossal duct cysts. They can develop anywhere along the thyroid's migratory path between the mouth and the inferior neck. They frequently manifest as midline neck cysts near to the hyoid bone.