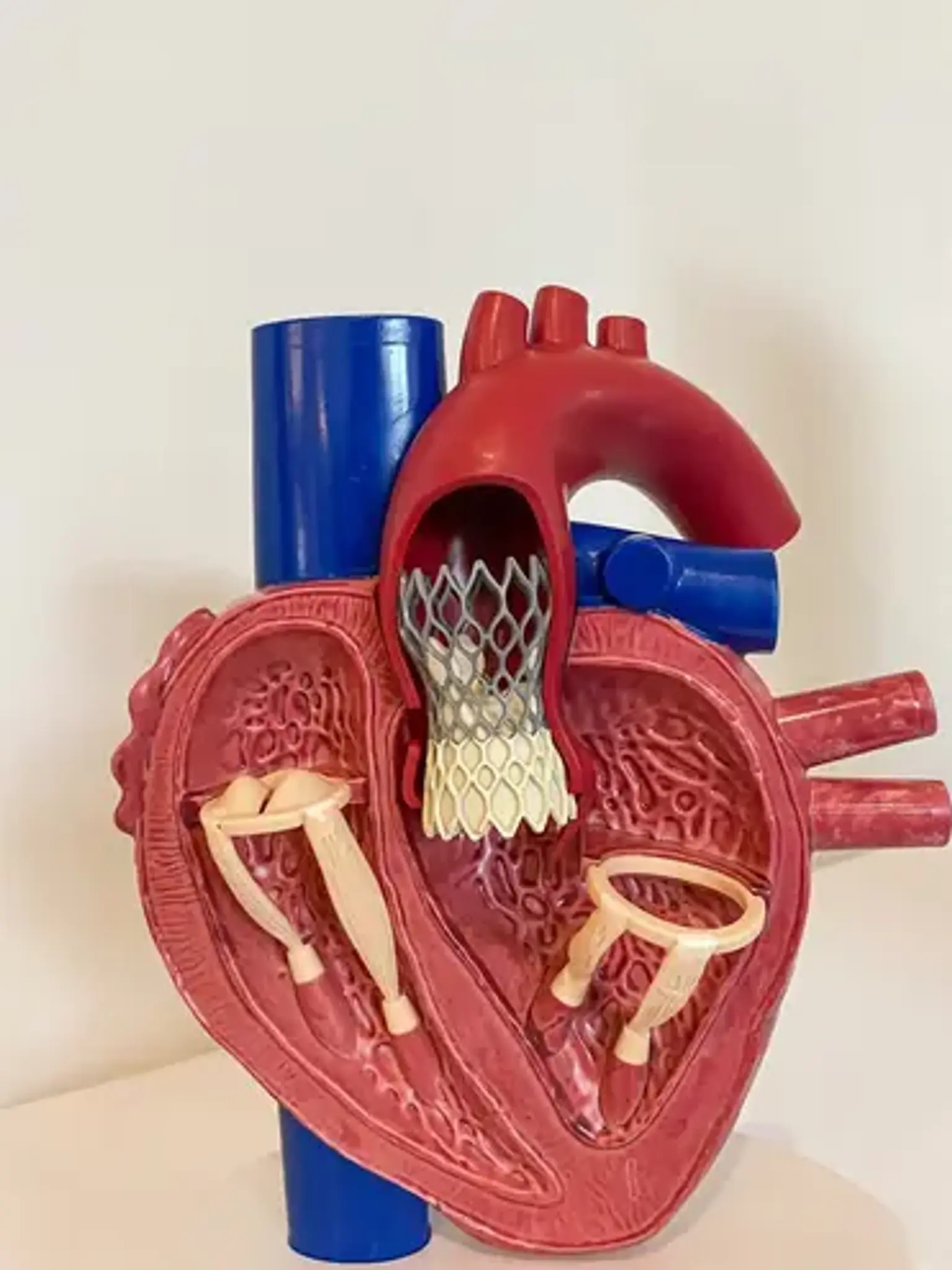
Transcatheter Aortic Valve Implantation (TAVI)
Overview
A failing aortic valve is replaced with an artificial one during transcatheter aortic valve implantation (TAVI), also known as transcatheter aortic valve replacement. This operation replaces a heart valve less invasively than the conventional open-heart surgery approach. As a result, TAVI is frequently chosen for patients who are at high risk for surgical problems, even though it is still a major procedure with potential risks. Additionally, TAVI is increasingly being considered for patients who don't have these preoperative concerns.