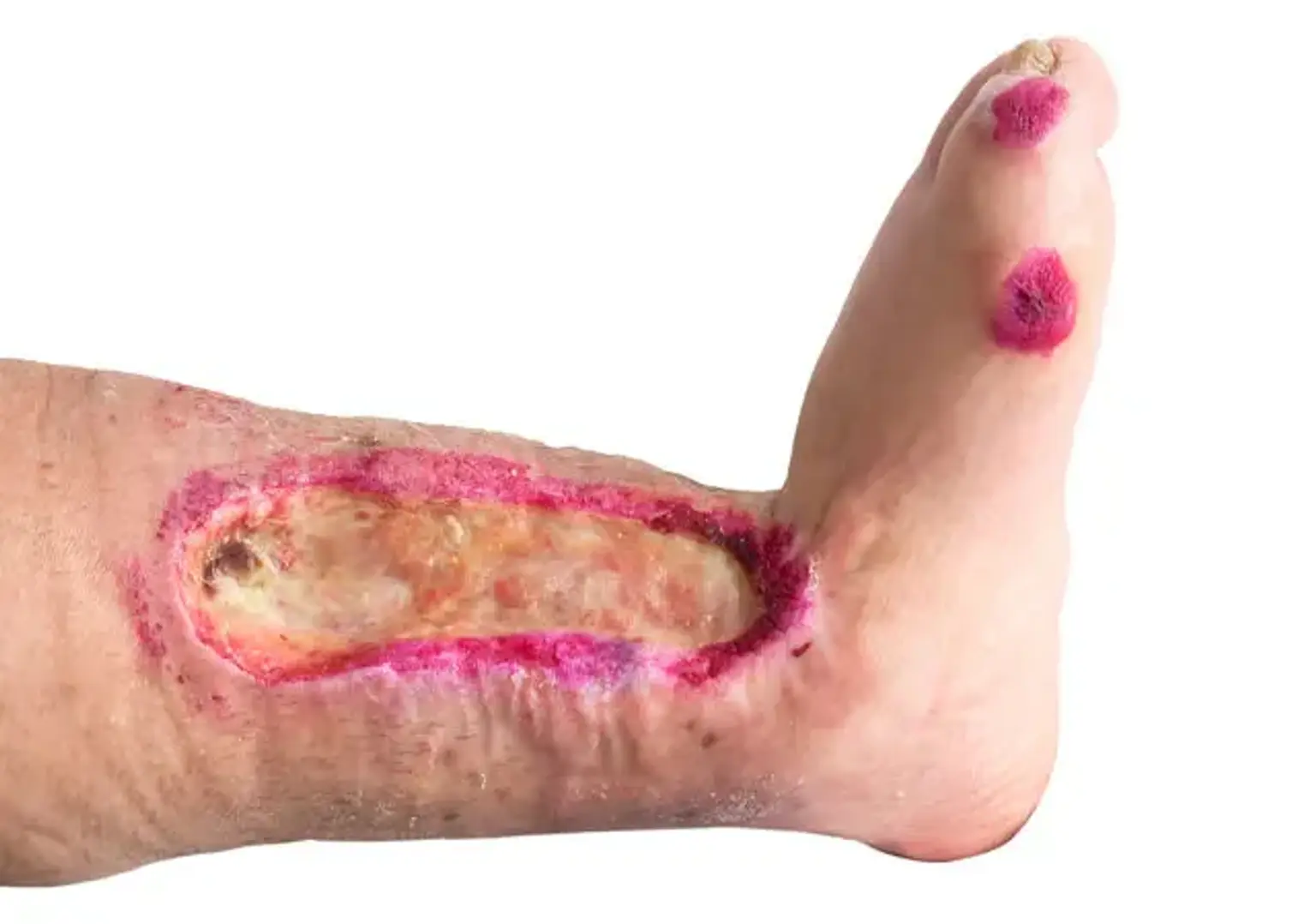
Trophic ulcer
Overview
Lower limb trophic ulcers afflict around 1–1.3% of the population and are the most serious and unpleasant consequence of chronic venous insufficiency. Although the pathophysiology of trophic ulcers is unknown, sufficient oxygen transport to tissues is undeniably important in wound healing. Hyperbaric oxygenation can now be used in patients with difficult-to-heal wounds thanks to recent technology improvements.
Though the general care of all trophic ulcers would be similar, the management would have to be tweaked on a case-by-case basis based on the aetiology and pathophysiology of the lesion. Because each ulcer's pathophysiology is unique, knowing the pathology might aid us in better addressing the disease.