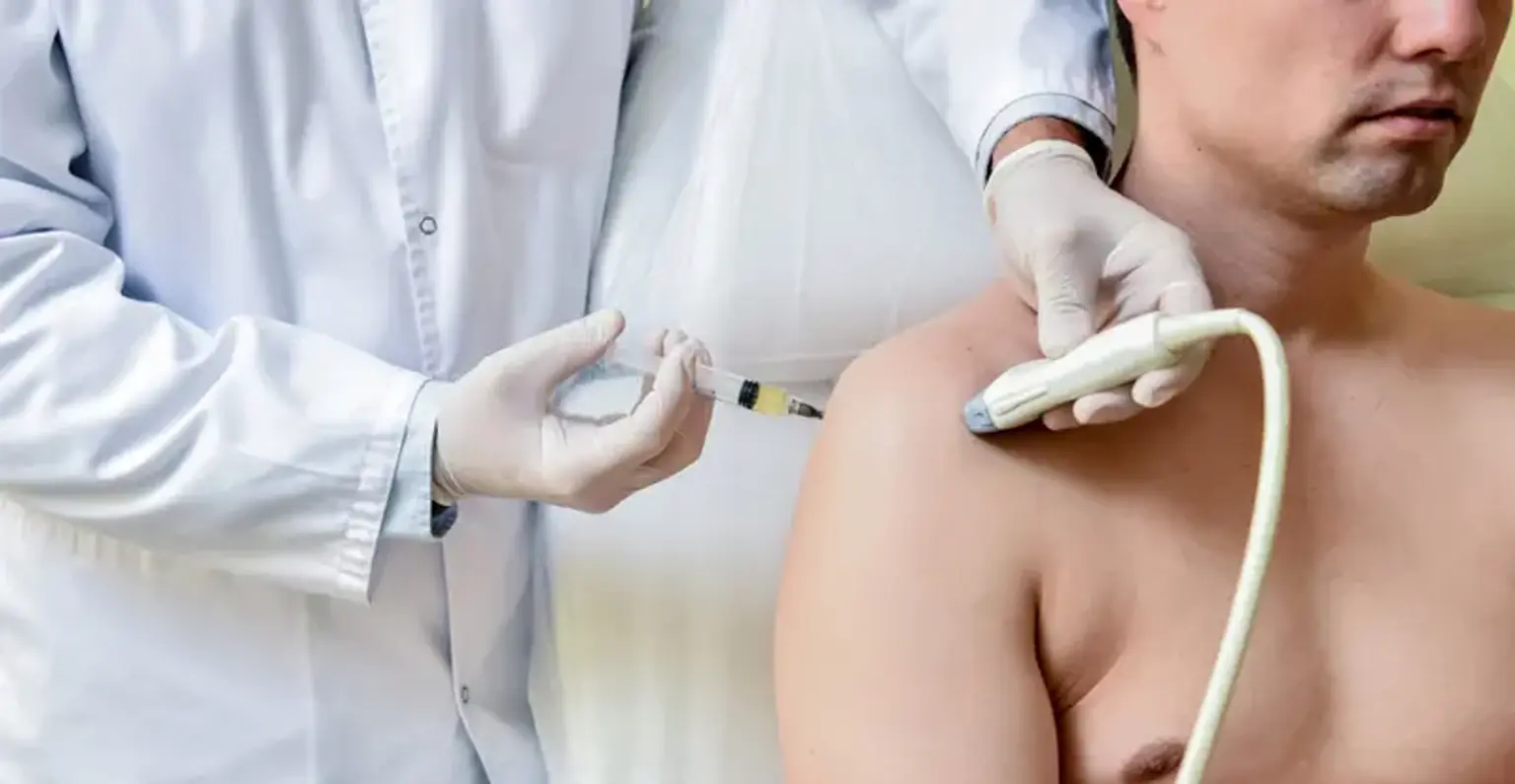
Ultrasound Guided Injections
Overview
Modern medical technology has made it easier and more accurate to diagnose and treat a wide range of orthopedic illnesses and injuries. Consider ultrasound-guided injections as an example. To treat a patient's symptoms, ultrasound-guided injections are typically utilized to administer drugs such as painkillers, anti-inflammatories, or joint lubricants (hyaluronic acid) into highly specific areas. Numerous of these injections occur at typical injury locations, such as joints like the knee, hip, or shoulder, and maybe a component of a more all-encompassing pain management strategy.