Overview
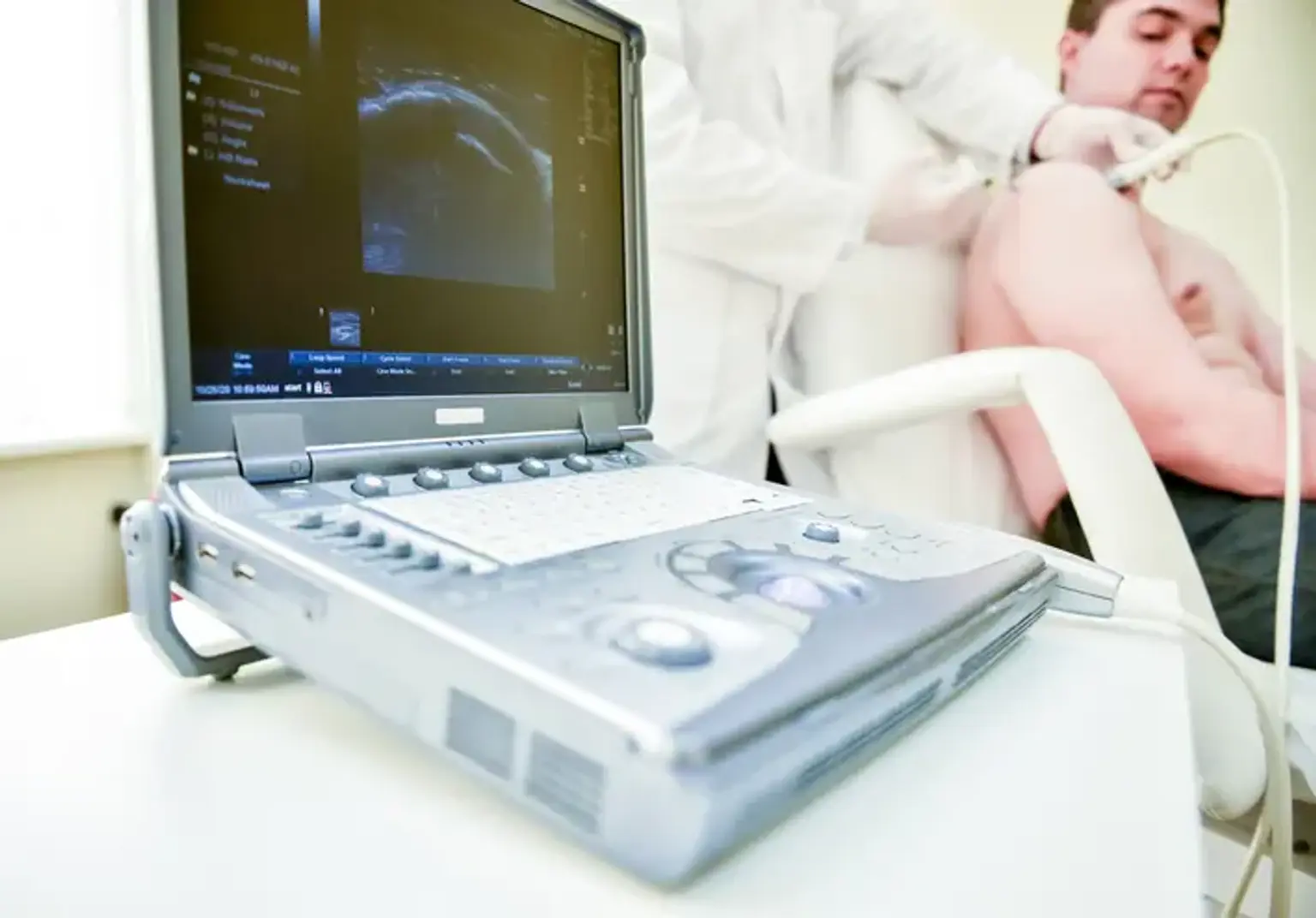
Ultrasound-guided joint injections are a modern technique used to treat joint pain and inflammation by delivering medication directly into the affected area with the help of real-time ultrasound imaging. This method allows healthcare professionals to precisely guide the needle, ensuring that the injection is administered exactly where it’s needed, which reduces the risk of complications and improves effectiveness.
The procedure is widely used to treat various joint conditions, such as arthritis, tendonitis, and bursitis, offering relief from pain and enhancing joint mobility. By using ultrasound imaging, the injection process becomes safer, as the physician can visualize the joint and surrounding tissues, avoiding vital structures like nerves and blood vessels.
Global Popularity and Growth
Ultrasound-guided joint injections have gained significant popularity worldwide due to their accuracy, safety, and effectiveness in treating joint pain. With the rise of minimally invasive techniques, patients and healthcare providers alike are turning to ultrasound guidance for pain management. This method has revolutionized the way joint injections are performed, offering a more targeted and controlled approach compared to traditional blind injections.
Globally, this technique has seen rapid adoption, especially in developed countries with advanced medical technology. Many patients now prefer ultrasound-guided injections due to their proven benefits, including fewer complications and better outcomes. As awareness increases, more healthcare centers are incorporating this technology into their practice, making the procedure more accessible.
What Are Joint Injections?
Joint injections are a medical procedure where medication, such as corticosteroids, hyaluronic acid, or platelet-rich plasma (PRP), is injected directly into a joint to reduce inflammation and alleviate pain. These injections are commonly used for conditions like arthritis, tendonitis, and other musculoskeletal disorders that affect the joints.
The primary purpose of joint injections is to provide immediate pain relief and improve joint function, particularly when other treatments, like oral medications or physical therapy, haven’t provided sufficient relief. Joint injections can also help delay or prevent the need for more invasive treatments, such as surgery.
How Ultrasound Works in Joint Injections
Ultrasound technology plays a crucial role in enhancing the precision and safety of joint injections. It uses sound waves to create real-time images of the joint and its surrounding structures, such as muscles, tendons, and ligaments. This live imaging allows healthcare providers to accurately position the needle and deliver the medication directly into the joint space.
The main advantage of ultrasound guidance is the ability to see the exact location of the needle in real-time, which reduces the chances of hitting unintended structures, such as nerves or blood vessels. It also ensures that the medication is injected in the most effective area, increasing the likelihood of a successful treatment. For patients, this means a safer procedure with less discomfort and a higher chance of pain relief.
Different Types of Joint Injections
Ultrasound-guided joint injections can involve various types of medications, each tailored to the patient's specific needs. The most common types include:
Corticosteroid Injections: These are anti-inflammatory drugs that help reduce swelling and pain in the joint. They are often used for conditions like arthritis and tendonitis.
Hyaluronic Acid Injections: These injections are used primarily for osteoarthritis. Hyaluronic acid is a substance naturally found in the synovial fluid of joints. Injections of hyaluronic acid help lubricate the joint and reduce pain and inflammation.
Platelet-Rich Plasma (PRP) Injections: PRP injections use the patient’s own blood, which is processed to concentrate platelets. This helps stimulate healing and tissue repair in damaged joints.
Each type of injection serves a different purpose, depending on the specific condition being treated. For example, corticosteroid injections are ideal for immediate relief from inflammation, while hyaluronic acid injections are often used to restore joint function and lubricate the joint for better mobility.
Indications for Ultrasound-Guided Joint Injections
Ultrasound-guided joint injections are particularly beneficial for patients with musculoskeletal disorders that affect the joints. Common conditions treated with ultrasound-guided injections include:
Arthritis: Both osteoarthritis and rheumatoid arthritis can cause severe joint pain. Injections of corticosteroids or hyaluronic acid help alleviate symptoms and improve mobility.
Tendonitis: This condition, caused by inflammation of the tendons, can be effectively treated with injections of corticosteroids or PRP to reduce pain and promote healing.
Bursitis: Inflammation of the bursae, the fluid-filled sacs that cushion the joints, can be treated with ultrasound-guided injections for faster relief.
Sports Injuries: Sprains, strains, and other sports-related injuries to joints often benefit from precise injections that target the affected area directly.
By using ultrasound to guide the injection, doctors can deliver the medication directly to the inflamed area, leading to faster and more effective relief.
Risks and Benefits of Ultrasound-Guided Joint Injections
Like any medical procedure, ultrasound-guided joint injections come with both benefits and risks.
Benefits:
Increased Precision: Ultrasound guidance allows for accurate needle placement, reducing the chances of complications.
Reduced Pain and Inflammation: Medications like corticosteroids and hyaluronic acid can significantly reduce pain and inflammation, improving joint function.
Minimal Recovery Time: The procedure is minimally invasive, allowing patients to return to normal activities quickly with few restrictions.
Risks:
Infection: While rare, any injection carries a small risk of infection.
Nerve or Blood Vessel Injury: If the needle is not accurately placed, there is a risk of damaging nearby nerves or blood vessels.
Temporary Discomfort: Patients may experience soreness or swelling at the injection site for a few days after the procedure.
Overall, the benefits of ultrasound-guided joint injections typically outweigh the risks, especially when performed by skilled practitioners.
Effectiveness and Expected Results
Ultrasound-guided joint injections are highly effective for many patients, particularly those suffering from arthritis or tendonitis. Success rates vary based on the condition being treated, but many patients experience significant pain relief and improved joint mobility.
Pain Relief: For conditions like arthritis, corticosteroid injections can offer relief within days, with effects lasting for weeks or even months.
Improved Joint Function: Hyaluronic acid injections are often used to restore lubrication and improve joint function, especially in osteoarthritis.
Long-Term Benefits: In some cases, the injections may delay the need for more invasive treatments, such as surgery.
Most patients begin to see improvements within 1-2 weeks after the injection, with some experiencing more dramatic results that last for several months.
Pre-Surgical Assessment and Preparation
Before undergoing an ultrasound-guided joint injection, it’s important to go through a pre-surgical assessment to ensure the procedure is right for you. Here’s what typically happens during the assessment:
Medical History Review: The healthcare provider will review your medical history, including any allergies, previous treatments, and existing health conditions like diabetes or autoimmune diseases that may affect the procedure.
Physical Examination: A physical examination of the affected joint will be conducted to assess the extent of inflammation, pain, and movement limitations.
Imaging Tests: In some cases, additional imaging, such as X-rays or MRIs, may be required to get a clearer picture of the joint condition before proceeding with the injection.
Pre-Injection Instructions: Your doctor may provide guidelines on what to do before the injection. For example, they may ask you to avoid taking blood thinners a few days before the procedure to reduce the risk of bleeding.
Proper preparation and a thorough assessment ensure the procedure is safe and effective, and that the right medication is chosen for your condition.
Long-Term Management of Joint Pain
Ultrasound-guided joint injections are often part of a broader, long-term strategy for managing joint pain and inflammation. While the injections can provide significant relief, maintaining joint health may require ongoing care and lifestyle changes.
Combining with Other Treatments:
Physical Therapy: After the injection, physical therapy can help strengthen the muscles surrounding the joint, reducing strain and promoting better joint function.
Medications: Oral anti-inflammatory drugs or disease-modifying drugs for arthritis may be prescribed in combination with injections for long-term pain management.
Weight Management: For weight-bearing joints like the knees and hips, maintaining a healthy weight can reduce stress on the joints and prevent further damage.
Regular monitoring and follow-up appointments with your healthcare provider are crucial to assess the success of the injections and adjust the treatment plan if needed.
Qualified Practitioners and Safety Protocols
The safety and effectiveness of ultrasound-guided joint injections depend largely on the skill and experience of the healthcare provider performing the procedure.
Qualified Practitioners:
Specialists: These injections should be performed by a trained physician, such as a rheumatologist, orthopedist, or sports medicine specialist, with expertise in musculoskeletal ultrasound.
Certification: Practitioners should be certified in ultrasound-guided injections, ensuring that they can accurately visualize the joint and surrounding structures.
Safety Protocols:
Sterility: The procedure is conducted in a sterile environment to minimize the risk of infection.
Real-time Imaging: Ultrasound allows the practitioner to monitor the needle’s position in real-time, reducing the risk of damaging nearby tissues, nerves, or blood vessels.
By ensuring that the procedure is done by a qualified practitioner and following strict safety protocols, patients can feel confident that they are receiving the best care possible.
Step-by-Step Guide to the Procedure
The process for an ultrasound-guided joint injection is typically quick, minimally invasive, and done on an outpatient basis. Here’s a step-by-step breakdown of what to expect:
Initial Assessment: Before the injection, the physician will conduct a thorough evaluation, which may include discussing medical history and performing physical tests to identify the cause of joint pain.
Ultrasound Setup: The patient is positioned comfortably, and an ultrasound probe is applied to the affected joint. The ultrasound gel is used to improve sound wave transmission and provide clear images of the joint.
Injection: Once the joint and surrounding structures are visualized, the physician will insert a needle through the skin into the joint space, guided by real-time ultrasound imaging. The medication is then injected directly into the joint.
Post-Injection Care: After the injection, the area may be massaged gently to help distribute the medication. Patients may experience a brief period of discomfort, but this usually subsides quickly.
The entire procedure typically takes 15-30 minutes, and most patients can resume normal activities shortly afterward, with some minor restrictions depending on the type of injection.
When to Expect Improvement
Improvement following an ultrasound-guided joint injection varies by individual and condition, but most patients begin to feel relief within a few days. For corticosteroid injections, pain relief can occur as early as 1-2 days after the procedure, with lasting effects typically seen within 1-2 weeks. For hyaluronic acid injections, results may take a bit longer, sometimes up to a week, but many patients experience significant improvements in joint mobility and function.
It's important to note that while the effects of the injection can last for several months, they may not provide permanent relief. In some cases, additional injections may be necessary to maintain benefits.
Advances in Ultrasound-Guided Joint Injections
The field of ultrasound-guided joint injections continues to evolve, with advancements in both technology and techniques improving patient outcomes.
Technological Advancements:
Higher-Resolution Ultrasound: Modern ultrasound machines provide clearer images, allowing for even greater precision in needle placement.
Needle Guidance Software: New software can further enhance the accuracy of needle insertion, making the process even safer and more effective.
Expanded Use:
Additional Joint Areas: Initially used mainly for large joints like the knee and shoulder, ultrasound-guided injections are now being successfully used for smaller joints, such as the wrists and elbows.
Combination Therapies: Researchers are exploring combining ultrasound-guided injections with other regenerative therapies like stem cell injections or PRP for enhanced healing and longer-lasting results.
As the technology continues to improve, ultrasound-guided joint injections will likely become even more precise, effective, and widely accessible.
Recovery Timeline and Aftercare
After the ultrasound-guided joint injection, recovery is typically quick. Most patients can return to their regular activities within a day or two, though some precautions should be taken.
First 24-48 Hours: Mild discomfort or swelling may occur at the injection site. Applying ice and resting the joint can help reduce these symptoms.
Activity Restrictions: Patients should avoid strenuous exercise or heavy lifting for a few days to allow the joint to heal.
Follow-Up: A follow-up appointment may be scheduled to assess the effectiveness of the injection and determine whether additional treatments are needed.
Overall, most people recover quickly, with full relief from symptoms often occurring within a few days to weeks.
What to Expect: A Patient’s Perspective
For many patients, ultrasound-guided joint injections offer a practical, low-risk option for managing chronic joint pain. However, the procedure can be intimidating if you’re unfamiliar with it. Here’s what you can expect from a patient’s perspective:
Before the Injection:
Patients typically experience a consultation to assess their condition and discuss potential benefits of the procedure. They may be nervous about the injection, but understanding that it’s a minimally invasive procedure can ease some of the anxiety.
During the Procedure:
Most patients report feeling little discomfort during the procedure. The ultrasound gel is applied to the skin, which is cold but not painful. The needle insertion itself is quick, and the real-time ultrasound helps ensure it’s accurate, reducing discomfort.
After the Injection:
Following the injection, some mild soreness may occur, but this is usually short-lived. Many patients are able to return to their normal activities within a day or two, though heavy lifting and strenuous exercise should be avoided for a short period.
For patients who have struggled with chronic joint pain, ultrasound-guided injections can be a life-changing treatment, providing long-lasting relief and a renewed ability to engage in daily activities.
Cost Considerations for Ultrasound-Guided Joint Injections
The cost of ultrasound-guided joint injections can vary depending on several factors, including the type of injection, location, and healthcare provider. On average, patients can expect to pay anywhere from $300 to $1,000 per injection. Insurance coverage may partially or fully cover the procedure, especially if it’s deemed medically necessary, but patients should check with their insurer for specific details.
Factors Influencing Cost:
Type of Injection: Corticosteroid injections are generally less expensive than PRP or hyaluronic acid injections.
Location: Costs may vary depending on whether the procedure is done in a hospital, outpatient clinic, or private practice.
Number of Injections: Some conditions may require multiple injections, which can increase the overall cost.
It’s important to weigh the cost against the benefits of the procedure, particularly for patients seeking long-term pain relief and avoiding more expensive, invasive surgeries.
Frequently Asked Questions (FAQs)
1. Are ultrasound-guided joint injections painful?
Most patients report minimal discomfort during the procedure. The needle insertion is brief, and ultrasound guidance reduces discomfort by ensuring precise placement.
2. How long does it take for the injection to work?
Pain relief can be felt within a few days, with full benefits often seen within 1-2 weeks, depending on the type of injection.
3. How long do the effects last?
Effects can last for several months, but the duration varies based on the type of injection and the individual’s condition.
4. Are there any side effects?
Minor side effects like swelling, bruising, or soreness at the injection site are common but usually short-lived. Serious side effects are rare.
5. How many injections can I get?
The number of injections depends on the condition and the type of medication used. Some patients may need periodic injections, while others may find long-lasting relief after just one.
Patient Testimonials and Success Stories
Many patients who undergo ultrasound-guided joint injections report significant improvements in their quality of life. For instance, a 55-year-old patient with knee osteoarthritis might share that after a corticosteroid injection, she was able to resume walking without pain after months of struggling with daily discomfort. Similarly, athletes recovering from tendon injuries often speak highly of PRP injections, praising their effectiveness in speeding up recovery.
These testimonials highlight the positive impact that precise, targeted treatments like ultrasound-guided joint injections can have on mobility, pain reduction, and overall well-being.
Conclusion
Ultrasound-guided joint injections offer a highly effective, minimally invasive solution for managing joint pain and inflammation. Whether you suffer from arthritis, tendonitis, or sports injuries, this procedure can provide lasting relief and improve your quality of life.
By offering increased precision, fewer complications, and faster recovery times, ultrasound-guided injections are becoming an increasingly popular choice among patients and healthcare providers alike. If you’re struggling with chronic joint pain, consider discussing this option with your healthcare provider to see if it’s the right treatment for your needs.