The clinical information regarding Rosacea in this article has been rigorously verified against the latest guidelines from the American Academy of Dermatology (AAD) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
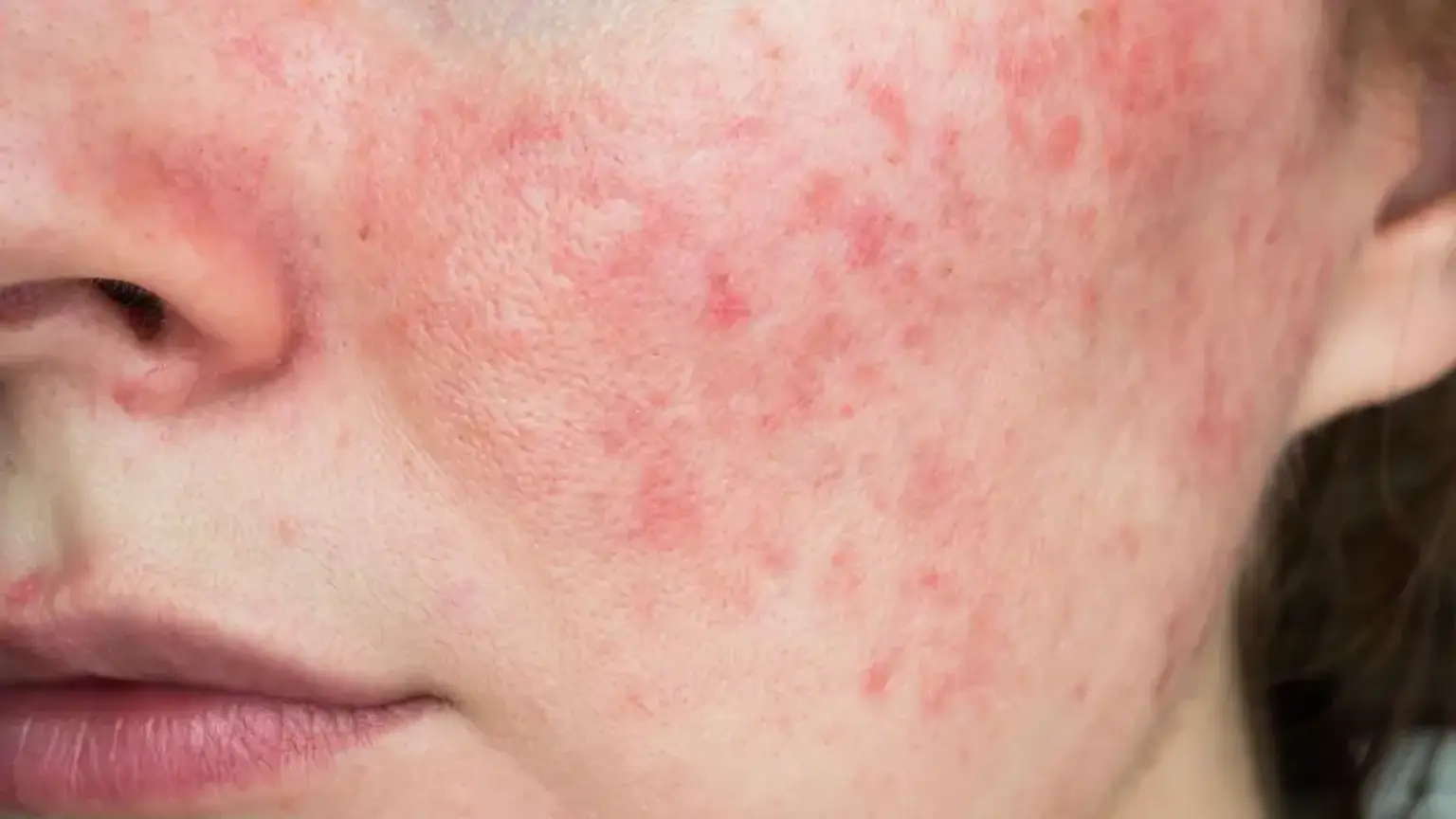
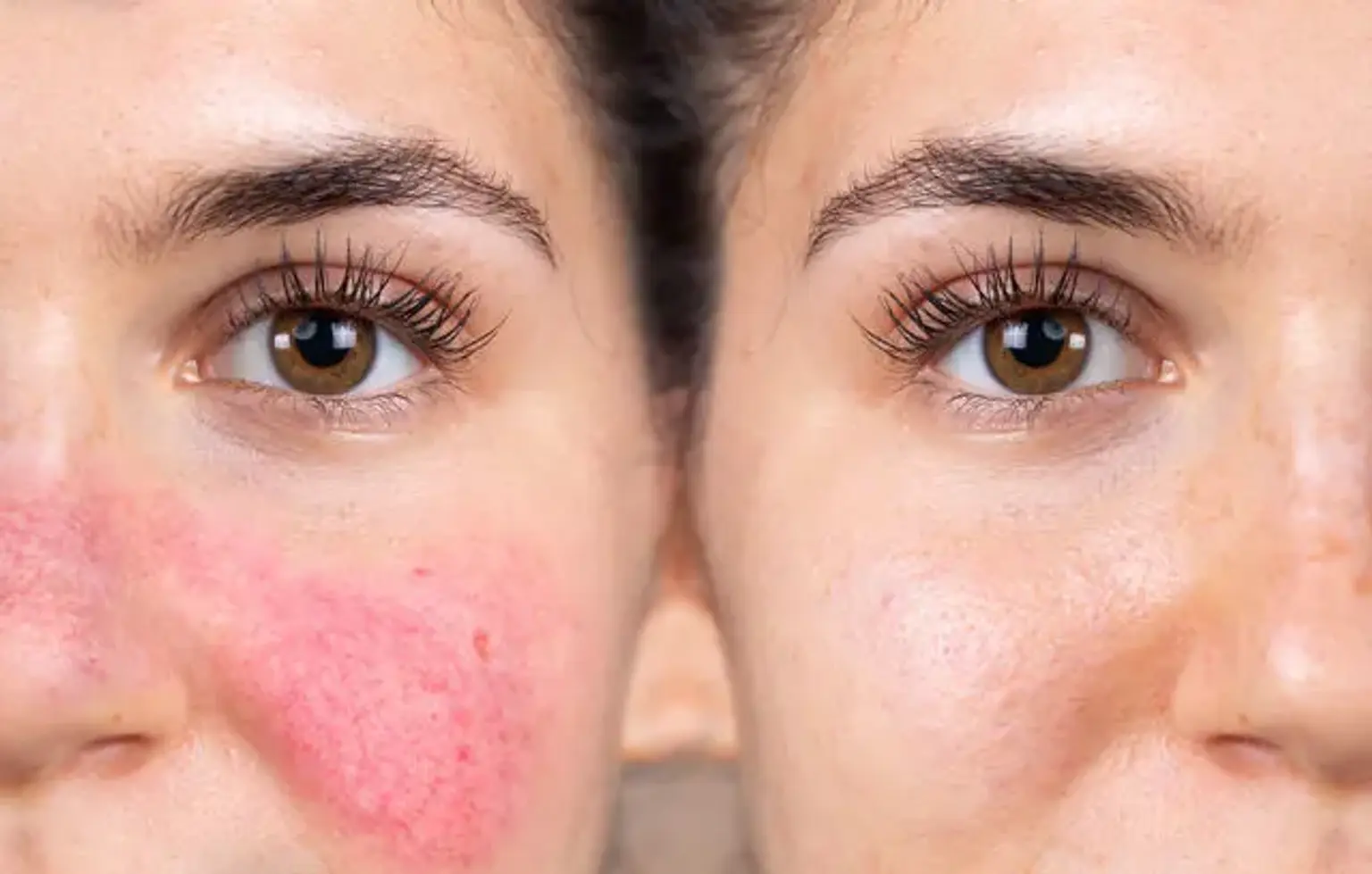
introductionRosacea is a chronic inflammatory skin condition that primarily affects the face, causing persistent redness, flushing, visible blood vessels, and sometimes bumps and pimples. It affects millions of people globally, yet it remains widely misunderstood. This guide provides a comprehensive overview of rosacea, offering clarity for those seeking to understand its causes, identify its symptoms, and explore effective management and treatment strategies.
What is Rosacea?
what-is-rosaceaRosacea is a long-term dermatological condition characterized by skin inflammation. It typically develops in adults, most commonly between the ages of 30 and 50, and is more prevalent in individuals with fair skin. The condition causes the small blood vessels in the face to become more visible, leading to a flushed or blushing appearance, particularly across the nose, cheeks, forehead, and chin. While there is no cure, various treatments can effectively control and reduce the signs and symptoms.
What are the four subtypes of rosacea?
what-are-the-four-subtypes-of-rosaceaRosacea presents in several ways, and a patient may experience symptoms of more than one subtype simultaneously. The condition is clinically categorized into four distinct subtypes based on the primary signs and symptoms.
Erythematotelangiectatic Rosacea (ETR): This is the most common subtype, characterized by persistent facial redness, flushing, and visible tiny blood vessels known as telangiectasia. The skin may feel sensitive, sting, or burn.
Papulopustular Rosacea (PPR): Often mistaken for acne, this subtype includes persistent redness along with bumps and pus-filled pimples (pustules). These breakouts are typically located in the central facial area.
Phymatous Rosacea: A rarer subtype that results in the skin thickening and developing a bumpy, swollen texture. When this affects the nose, it is called rhinophyma, causing the nose to appear enlarged and bulbous. This form is more common in men.
Ocular Rosacea: This subtype affects the eyes, causing them to appear bloodshot or watery. Symptoms can include a gritty or foreign body sensation, burning, stinging, dryness, itching, and light sensitivity. In some cases, ocular symptoms may appear before skin symptoms.
What are the most common triggers for a rosacea flare-up?
what-are-the-most-common-triggers-for-a-rosacea-flare-upThe exact cause of rosacea is unknown, but a combination of genetic and environmental factors is believed to be responsible. A key aspect of managing rosacea is identifying and avoiding personal triggers that cause flare-ups.
Common Triggers Include:
Sun Exposure: UV radiation is one of the most significant triggers for rosacea symptoms.
Emotional Stress: Anxiety, embarrassment, or high stress levels can induce flushing.
Weather Extremes: Hot weather, high humidity, cold, and strong winds can all provoke a reaction.
Food and Drink: Spicy foods, hot beverages like coffee and tea, alcohol (especially red wine), and foods containing cinnamaldehyde like cinnamon, chocolate, tomatoes are frequent culprits.
Intense Exercise: Strenuous physical activity can lead to overheating and flushing.
Certain Skincare Products: Products containing alcohol, witch hazel, fragrance, menthol, or exfoliants can irritate sensitive, rosacea-prone skin.
Medical Conditions: A fever, cough, or hot flashes associated with menopause can trigger flare-ups.
Demodex Mites: These microscopic mites are a natural part of the human skin microbiome, but they have been found in greater numbers on the skin of people with rosacea, suggesting they may play a role in the inflammation.
How is rosacea officially diagnosed by a dermatologist?
how-is-rosacea-officially-diagnosed-by-a-dermatologistA definitive diagnosis for rosacea is made through a clinical evaluation by a dermatologist. There is no single blood test or skin biopsy to confirm the condition. The diagnostic process involves a thorough physical examination of the skin and a detailed discussion of your personal and medical history.
A dermatologist will typically:
Examine Your Skin: They will look for the characteristic signs of rosacea, such as persistent central facial redness, visible blood vessels, papules, and pustules.
Discuss Your Symptoms: You will be asked about the history of your symptoms, including when they started, how often you experience flushing, and if you have any stinging or burning sensations.
Identify Triggers: The doctor will help you identify potential triggers by discussing your diet, lifestyle, and skincare routines.
Rule Out Other Conditions: The dermatologist must differentiate rosacea from other skin conditions that can cause similar symptoms, such as acne, lupus, seborrheic dermatitis, or an allergic reaction.
What is the most effective treatment for rosacea redness and bumps?
what-is-the-most-effective-treatment-for-rosacea-redness-and-bumpsThe most effective treatment for rosacea is highly individualized and often involves a combination of prescription therapies, professional procedures, and lifestyle modifications. A dermatologist will recommend a plan based on your specific subtype and symptom severity.
Prescription Topical and Oral Medications
prescription-topical-and-oral-medicationsTopical Creams and Gels: These are often the first line of defense.
Metronidazole: An antibiotic and anti-inflammatory cream or gel that reduces redness and bumps.
Azelaic Acid: A gel or foam that helps unclog pores, reduce inflammation, and decrease the production of keratin.
Ivermectin: A cream that kills Demodex mites and reduces inflammation.
Brimonidine and Oxymetazoline: Gels specifically designed to reduce persistent facial redness by constricting blood vessels.
Oral Medications:
Antibiotics: Low dose oral antibiotics, particularly Doxycycline, are used for their anti-inflammatory properties to control bumps and pustules, not to kill bacteria.
Isotretinoin: In severe, resistant cases of papulopustular rosacea, this powerful oral medication may be prescribed off-label.
Professional In-Clinic Procedures
professional-in-clinic-proceduresLaser and Light-Based Therapies: These are highly effective for treating persistent redness and visible blood vessels telangiectasia.
Pulsed Dye Laser (PDL): Considered a gold standard for reducing redness and visible vessels. It uses a concentrated beam of light to target and collapse the blood vessels without damaging surrounding skin.
Intense Pulsed Light (IPL): Uses broad-spectrum light to target hemoglobin in the blood vessels, reducing redness and improving overall skin tone. Multiple sessions are typically required for optimal results.
Microneedling RF: Devices like the Secret Laser combine microneedling with radiofrequency energy to improve skin texture and reduce inflammation associated with some forms of rosacea.
What skincare ingredients should be avoided with rosacea?
what-skincare-ingredients-should-be-avoided-with-rosaceaProper skincare is fundamental to managing rosacea. Using gentle products and avoiding known irritants can prevent flare-ups and calm sensitive skin.
Key Ingredients to Avoid:
Alcohol (often listed as SD alcohol or denatured alcohol)
Fragrance/Parfum
Menthol, Camphor, and Peppermint
Eucalyptus Oil
Witch Hazel
Sodium Lauryl Sulfate (SLS)
Harsh physical scrubs or chemical exfoliants like high-concentration Glycolic Acid.
Instead, opt for hydrating and soothing ingredients like ceramides, hyaluronic acid, niacinamide, and thermal spring water. Daily use of a broad-spectrum mineral sunscreen like zinc oxide or titanium dioxide with an SPF of 30 or higher is non-negotiable.
"For years, I thought the constant burning flush on my cheeks was just something I had to live with. Getting an actual diagnosis of rosacea was a huge relief. It gave my problem a name and, more importantly, a clear path to managing it. Avoiding my triggers and using the right laser treatments has given me my confidence back." – an anonymous patient, United States.
When should I see a doctor for facial redness?
when-should-i-see-a-doctor-for-facial-rednessYou should schedule an appointment with a dermatologist if you experience persistent facial redness that doesn't go away. Early diagnosis and treatment are crucial for controlling symptoms and preventing the condition from progressing.
Seek professional medical advice if you notice:
Flushing or blushing that becomes more frequent or lasts longer.
Redness on your cheeks, nose, forehead, or chin that does not fade.
The appearance of small, visible blood vessels on your face.
Acne-like bumps that don't respond to over the counter acne treatments.
Stinging, burning, or sensitivity in your facial skin.
Any eye symptoms like persistent dryness, grittiness, or redness.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaSouth Korea is renowned for its advanced dermatological clinics, offering cutting-edge laser technologies and expert care for conditions like rosacea.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Advanced Lifting & Facial Contouring | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | Specialized Plastic Surgery & Anti-aging | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Comprehensive Dermatology, Lifting & Injectables | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Facial Plastic Surgery (Eyes, Nose, Face) | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | Anti-aging Dermatology & Body Contouring | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology | Comprehensive Dermatology & Laser Treatments | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | Advanced Dermatology & Aesthetic Procedures | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Premium Lifting, Skin Boosters & Injectables | Gangnam-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaThe following table outlines common dermatological procedures available in South Korea that are either used to treat rosacea or address general skin health and aesthetics. Costs are estimates and can vary by clinic and the specifics of the treatment plan.
Treatment/Procedure Name | Duration | Hospitalization? | Avg.Cost (USD) in S. Korea | Contact |
|---|---|---|---|---|
Laser Treatment (for Rosacea, e.g., PDL/IPL) | 20-30 mins | Not Needed | $250 - $500 | |
Pigmentation & Whitening (Laser Toning) | 20-40 mins | Not Needed | $200 - $450 | |
Secret Laser (Microneedling RF) | 30-60 mins | Not Needed | $400 - $700 | |
Hydrogen Toning | 45-60 mins | Not Needed | $150 - $300 | |
Rejuran Healer | 20-30 mins | Not Needed | $300 - $550 | |
Juvelook | 30-45 mins | Not Needed | $450 - $800 | |
Thermage FLX | 45-90 mins | Not Needed | $1,500 - $3,000 | |
Ulthera | 30-90 mins | Not Needed | $1,200 - $2,800 | |
Titanium Lifting | 40-60 mins | Not Needed | $800 - $1,500 | |
Skin Botox – Full Face | 20-30 mins | Not Needed | $350 - $600 |
Frequently Asked Questions About Rosacea
frequently-asked-questions-about-rosacea1. Can rosacea be permanently cured or only managed?
1.-can-rosacea-be-permanently-cured-or-only-managedRosacea cannot be permanently cured, but it can be effectively managed to the point where symptoms are minimal or completely controlled. Consistent treatment, adherence to a gentle skincare routine, and diligent trigger avoidance are key to long-term remission.
2. Is rosacea hereditary?
2.-is-rosacea-hereditaryThere is a strong genetic component to rosacea. You are more likely to develop the condition if you have a family history of rosacea or come from certain ethnic backgrounds, particularly Celtic or Scandinavian ancestry.
3. Can diet really affect my rosacea?
3.-can-diet-really-affect-my-rosaceaYes, diet can significantly impact rosacea for many individuals. While triggers are personal, common culprits include spicy foods, alcohol, hot drinks, and foods high in histamine or cinnamaldehyde. Keeping a food diary can help you identify your specific dietary triggers.
4. Does rosacea get worse with age?
4.-does-rosacea-get-worse-with-ageIf left untreated, rosacea symptoms can become progressively more severe over time. What starts as intermittent flushing can evolve into persistent redness, visible blood vessels, and papulopustular breakouts. This makes early intervention by a dermatologist essential.
5. Is rosacea related to acne?
5.-is-rosacea-related-to-acneWhile Papulopustular Rosacea is often called acne rosacea, it is a distinct condition. Unlike acne, rosacea is not caused by clogged pores and does not feature blackheads. It is an inflammatory vascular condition, whereas acne is a disorder of the hair follicle and sebaceous gland.
6. Can makeup make rosacea worse?
6.-can-makeup-make-rosacea-worseYes, certain makeup products can irritate rosacea prone skin and trigger a flare-up. It is best to choose mineral-based, fragrance free cosmetics. Always remove makeup gently at the end of the day and ensure you are using clean brushes and sponges.
7. What's the difference between rosacea and just having sensitive skin?
7.-what's-the-difference-between-rosacea-and-just-having-sensitive-skinWhile rosacea prone skin is inherently sensitive, not all sensitive skin is due to rosacea. Sensitive skin is a general term for skin that is easily irritated. Rosacea is a specific medical diagnosis characterized by a distinct set of clinical signs, such as persistent central facial erythema and telangiectasia.
Take Control of Your Rosacea: Get Your Personalized Treatment Plan
take-control-of-your-rosacea:-get-your-personalized-treatment-planLiving with rosacea doesn't mean resigning yourself to constant redness and discomfort. With expert diagnosis and access to today's advanced treatments, you can effectively manage your symptoms and restore your skin's health. The journey begins with a professional consultation. We provide a seamless, transparent process, connecting you with top-tier dermatologists in South Korea and providing a dedicated Care Manager for end-to-end support. And Start Your Confidential Inquiry with CloudHospital to receive a personalized plan and take the first step towards clearer, calmer skin.