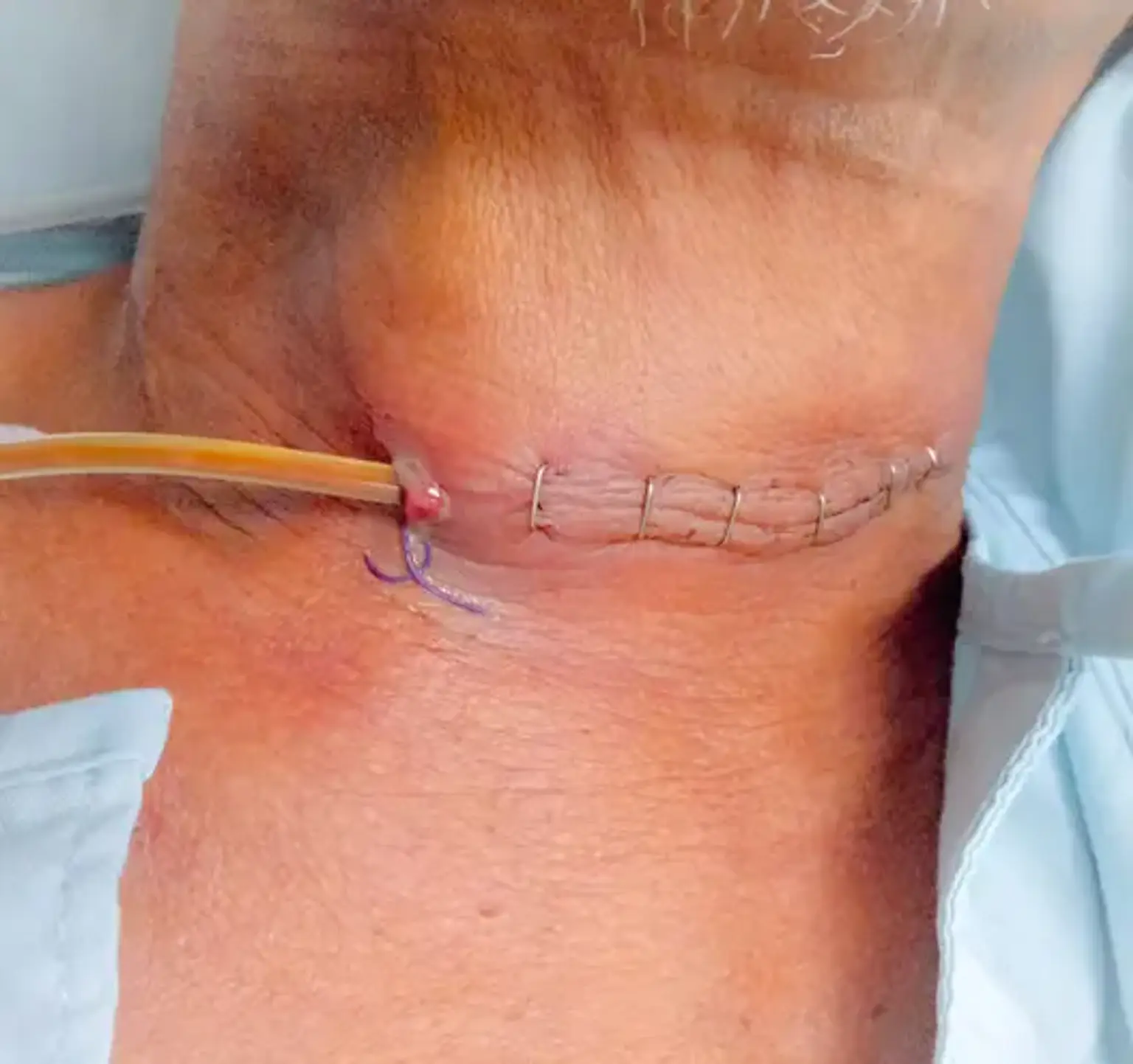
Cervical Esophagostomy
Overview
Many diseases are characterized by an inability to eat and a lack of appetite. Malnutrition, which is known to impair immune function and wound healing, can quickly result from these disorders. Treatment for sick people who are unable to consume enough food to meet their nutritional needs typically includes nutritional support.
Nutritional support can save lives, or at least, it can accelerate the process of healing, getting out of the hospital, and getting back to normal activity. Nutritional supplementation may also benefit the patient's wellbeing if appetite is present but oral eating is not possible by merely lessening the unpleasant feeling of hunger. Patients can get parenteral feeding, but this requires the use of pricey, sterile admixtures containing only pure nutrients, and problems are not uncommon.
To lower morbidity, mortality, and costs, it is currently advised in human medicine to avoid parenteral nourishment whenever the patient can be fed by the enteral route. It is even more appealing to use the enteral method in the case of big patients because of some unique features, like their big body size, complex gastrointestinal environment, and gastrointestinal tract that is adapted to frequent large meals. It is possible to deliver a small amount of widely used human feed with a significant amount of fiber for a few days using a large-bore nasogastric tube.