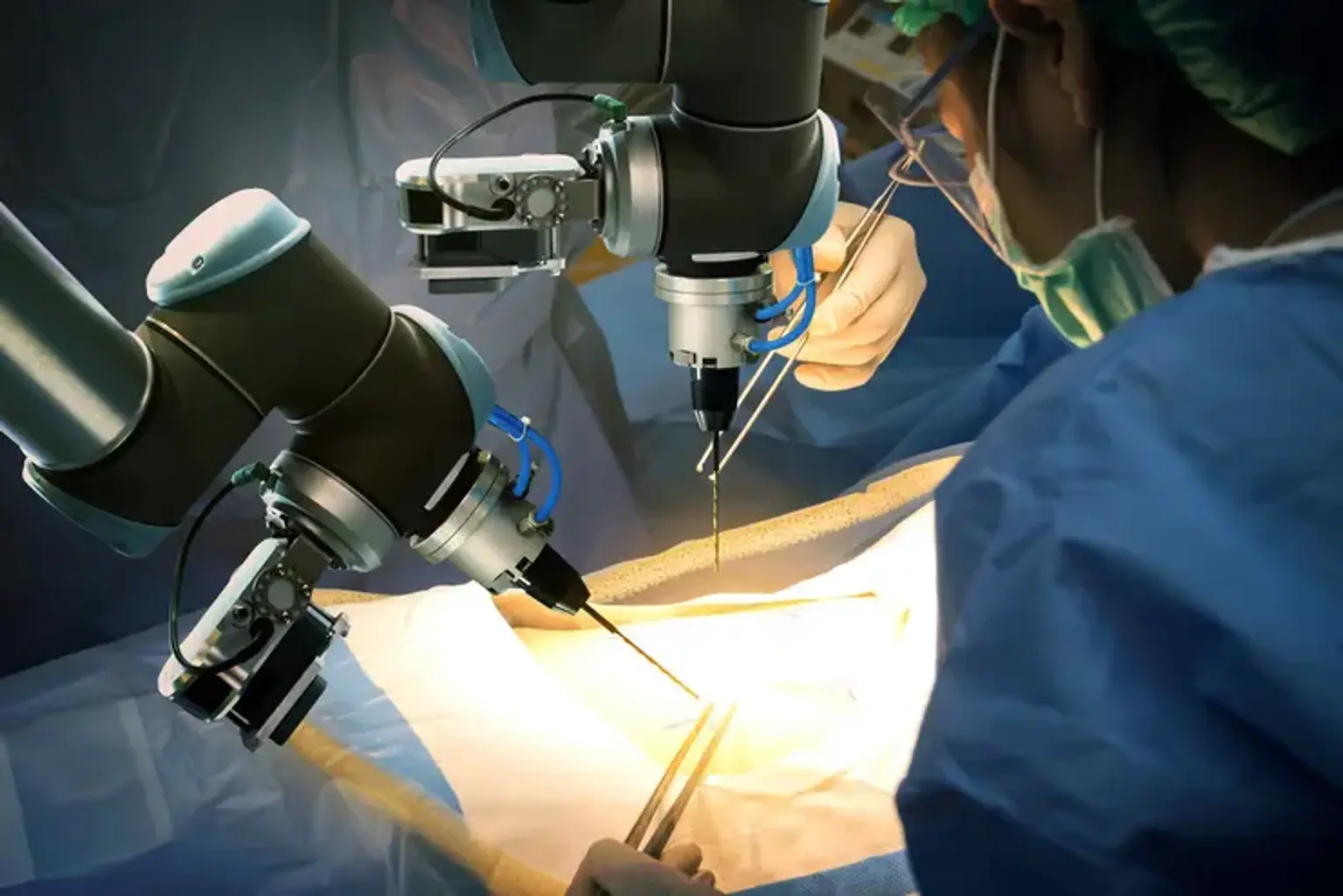
Gastrointestinal Robotic Surgery
There have been two major developments in the treatment of gastrointestinal cancer in the last 20 years. The evidence-based standardization of anticancer medication treatment, which was based on the outcomes of many research (including randomized controlled trials) conducted around the world, is one example of a breakthrough. The spread of minimally invasive surgery, such as laparoscopic and thoracoscopic surgery, is another breakthrough. Endoscopic surgery, such as laparoscopic surgery and thoracoscopic surgery, is increasingly commonly utilized for gastrointestinal cancers, including esophageal cancer, stomach cancer, hepatopancreatobiliary cancer, and colorectal cancer. However, unlike the above-mentioned standard of anticancer drug treatment, the expansion of minimally invasive surgery is not supported by solid evidence. Surgical techniques and skills utilized in gastrointestinal cancer surgery vary depending on the facility and surgeon. As a result, unlike the outcomes of anticancer drug therapies, it is extremely difficult to compare outcomes such as surgery's curability and complications.
Robotic surgery in gastrointestinal surgery is becoming more popular as one of the most promising types of minimally invasive procedures. A robot-assisted surgery system is used to perform robotic surgery in the area of gastrointestinal diseases.
What is Robotic Surgery?
Robotic surgery is a form of minimally invasive surgery in which surgeons utilize very tiny surgical tools that are inserted into the patient's body through a series of small cuts.
These devices are installed on three robotic arms, giving the surgeon the greatest range of motion and precision while performing the treatment. A fourth arm carries a high-definition, three-dimensional camera that improves visualization by tenfold magnification of the body's tissue and structures and assists the surgeon throughout the procedure.
After scaling each action down to size, the robot translates the surgeon's hand, wrist, and finger movements to direct each device in real-time. A one-inch movement, for illustration, can be scaled down to a quarter-inch, allowing for remarkable surgical accuracy and control.
Robotic Surgery Advantages
One of the key benefits is that surgery can be performed with minimal incisions.
The following are some of the other advantages of robotic surgery:
- Increased precision. The actions of the robotic arm are more precise than those of a human hand. And they have a wider range of movement. Instruments can be rotated in tight spaces in directions that aren't achievable otherwise.
- Better visualization. A sophisticated camera delivers magnified, high-definition pictures of the surgery area, allowing for better visibility. It also has 3D imaging capabilities that are superior to those of the naked eye.
- Ability to do surgery inside the body. Small tools enable surgeons to perform steps of the procedure within your body where they would have had to make a considerably larger incision to do that aspect of the procedure outside of your body in the past.
Robotic Surgery Disadvantages
The following are a few of the disadvantages of gastrointestinal robotic surgery:
- Only available in facilities that can pay for the technology and have surgeons who have undergone special training.
- If difficulties arise, your surgeon may need to proceed to an open operation with larger incisions. These include scar tissue from past procedures, which makes robotic technology challenging to perform.
- Nerve injury and compression are possible side effects.
- Robotic malfunction is possible but highly uncommon.
Robotic Heller Myotomy
Achalasia cardia is a neurodegenerative motility condition characterized by decreased esophageal peristalsis and loss of function of the lower esophageal sphincter. Achalasia treatment options now available are unable to prevent or reverse neurodegeneration. The tone of the lower esophageal sphincter can be reduced (through various pharmacological treatments and/or botulinum toxin injection) or obliterated (by endoscopic balloon dilatation and/or surgical surgery) in patients with achalasia.
The option of removing the lower esophageal sphincter dates back to Sir Thomas Willis' whale-bone dilation trials in the 1600s. The usage of the first balloon dilatation in the 1880s, Ernest Heller's description of surgical myotomy, the inclusion of antireflux procedures in myotomy, the advent of minimally invasive surgery, per-oral endoscopic myotomy (POEM), and the latest robotic surgical procedures continued the historical development.
Because of its advantages over traditional minimally invasive approaches, robotic surgery is likely to become the primary option for achalasia surgery.
Robotic Colectomy
Robotic colorectal surgery has been found to improve cancer management and clinical results. It has a lower risk of infection, less postoperative pain, a faster recovery of bowel function, shorter hospital stays, and a faster complete recovery than traditional open surgery.
The colon, also known as the large intestine, is located at the bottom of the intestines. A colectomy, also known as a colon resection, is a surgical procedure that is used to treat colon cancer, infections, and inflammatory bowel disease (ulcerative colitis and Crohn's disease). Only a portion of the colon is removed during a partial colectomy. A total colectomy involves the removal of the entire colon.
When a surgeon does a colectomy to treat a malignant tumor, he or she must remove the tumor as well as the vascular and lymphatic structures that are related to that section of the colon. This operation may be curative depending on the stage of the malignancy.
An open colectomy is done with one long incision through the center of the abdomen, whereas a robotic colectomy is conducted with multiple small incisions. A robotic colectomy also has the advantages of a shorter hospital stay, less postoperative pain, and a quicker recovery time. With robotic surgery, the gastrointestinal tract recovers more quickly, allowing patients to start eating sooner. Additionally, after a robotic colectomy, it is occasionally possible to avoid the use of narcotic pain medications. In comparison to conventional open surgery, which takes 4-6 weeks to recover from, the robotic technique takes 2-3 weeks.
Robotic Rectal Resection
Rectal resection is a cancer operation that removes part or all of the rectum (the lower part of the colon). Rectal cancer operation is one of the most difficult types of surgery due to the limited area available within the pelvis. To see and remove the malignancy in traditional open surgery, the surgeon must make a large cut along the middle of the patient's abdomen. Due to the ability to see a three-dimensional picture of the pelvis, robotic-assisted surgery requires the doctor to make multiple small incisions. Furthermore, robotic tools have a significantly greater range of rotation than human hands.
Less blood loss, less postoperative pain, reduced hospital stays, and faster recovery are all benefits of the robotic operation for the patient. A robotic rectal resection usually takes 2-3 weeks to heal from, compared to 4-6 weeks for traditional open surgery.
Robotic Cholecystectomy
The gallbladder is removed with the help of a robot during a robotic cholecystectomy. The doctor has full control over the robot. This surgery, like the laparoscopic method, involves small incisions.
Robotic cholecystectomy is a very safe procedure when performed by a surgeon who is well-trained and skilled in the use of robotic surgery. The robot's developer has a strict training program in place and is actively involved in its use. This contributes to the safety of robotic surgery.
In a typical operating room, a robotic cholecystectomy is performed under general anesthesia. This procedure is now performed as an outpatient procedure. The surgery takes about one hour to finish.
The time it takes for a patient to recover from a robotic cholecystectomy varies depending on the patient, although it is usually only two to four days at home. In many cases, narcotic pain medication is not required. After the gallbladder is removed, people can eat a regular diet in the long term.
Robotic Nissen Fundoplication
The Nissen fundoplication procedure has a long history of excellent success and can be performed on practically any severe GERD patient. It is the most common fundoplication procedure in the world. To prevent acid reflux, the surgeon wraps the upper part of the stomach around the esophagus during the procedure.
Instruments and a fiber-optic camera are manipulated through multiple tiny incisions during robotic-assisted surgery. On a video screen, the surgeon may see images from inside the body through the camera.
In more than 90% of patients with typical GERD symptoms, this surgery successfully resolves their reflux problems (heartburn, regurgitation, dysphagia). Around 70% of people with GERD airway symptoms have their symptoms resolved successfully.
A surgeon can conduct a wide range of treatments with small 1-2 cm incisions using robotic-assisted visualization, flexibility, precision, and control. The surgeon guides the robotic arms to perform the procedure while sitting at a console in the surgical suite. The surgeon's natural hand, wrist, and finger movements are smoothly and directly converted from controls at the console to surgical tools within the patient by the robot.
Robotic Gastrectomy
Laparoscopic surgery for gastrectomy has become an alternate option for early gastric cancer 25 years after the first laparoscopic gastrectomy with lymph node dissection was published. Meanwhile, the Korean Laparoendoscopic Gastrointestinal Surgery Study Group (KLASS)-02 trial recently showed that laparoscopic distal gastrectomy with D2 lymph node dissection is also useful in terms of short-term results for advanced gastric cancer, and continuing randomized clinical trials developed to evaluate the long-term oncologic outcomes of laparoscopic gastrectomy are expected to expand the indications of minimally invasive surgery for gastric cancer.
Four small incisions are made during a robotic-assisted gastrectomy procedure: one incision near the patient's belly button and three incisions in the upper abdomen.
The doctor separates the stomach with cancer from adjacent organs such as the transverse colon, liver, spleen, and pancreas in a partial gastrectomy, which is widely used to treat gastric cancer. The feeding blood vessels and lymph nodes, as well as the relevant stomach segment, are identified and transected. The lower end of the stomach is joined to the lower end of the esophagus if the top section of the stomach is removed. The upper half of the stomach is connected to the small intestine if the lower part of the stomach is excised. Typically, the connection is made with a stapling tool or by hand sewing with robotic devices. Feeding tubes or drains are inserted.
The stomach is mobilized during gastric fundoplication, especially around the lower esophagus and spleen. The upper section of the stomach and the esophagus are wrapped and sutured with the stomach fundus.
Robotic Pancreas Surgery
Robotic pancreas surgery is a minimally invasive procedure that can only be done on a small number of individuals. It alleviates part of the discomfort that comes with traditional open surgery. Don't panic, surgeons, not robots, perform robotic surgery. The surgeons utilize the operating robot as an instrument to make tiny incisions and cut and stitch at angles that are impossible to achieve with human hands. The procedure is often conducted with three or four half-inch or one-inch incisions, avoiding a large wound for the patient. The tumor is removed using fine surgical instruments guided by a surgical robot. Robotic surgery has essentially replaced laparoscopic surgery.
Robotic surgery is frequently favored over laparoscopic surgery because it overcomes laparoscopy's inherent limitations (long straight tools that do not flex). Many studies have proven that robotic pancreatectomy is a safe surgery for both benign and malignant causes since its inception in the early 2000s. In comparison to open pancreatectomy, robotic pancreatectomy has shown a reduction in morbidity, with a lower incidence of wound complications and a shorter postoperative stay, allowing for improved recovery protocols and early adjuvant treatment.
Pancreas surgery is difficult, and several published studies have found that it is safest to have it done in a specialized center with a lot of experience. As a result, doctors advise that pancreas surgery be done by a specialist who is experienced with conventional pancreas tissue handling techniques, particularly at high-volume centers.
Robotic Ventral Mesh Rectopexy
Ventral Mesh Robotic Rectopexy is a da Vinci-assisted treatment that involves mobility of the anterior part of the rectum to the pelvic floor and bio-dissolvable mesh attachment of the anterior of the rectum and pelvic floor to the bony sacral promontory. The rectum is stretched and its tubular shape is restored.
The nerves that enter the rectum from the back and sides are protected in this procedure, which mobilizes the rectum only from the anterior and right sides. The preservation of nerves in the posterior part of the rectum is thought to improve rectal function and emptying while also lowering the likelihood of hindgut neuropathy and constipation. The biodegradable mesh is anticipated to have a lower recurrence rate than sutured rectopexy, while also avoiding the long-term consequences of permanent mesh infection and erosion.
Due to the enhanced simplicity with which suturing may be accomplished with the robot within the limited constraints of the bony pelvis, robotic ventral mesh rectopexy with the da Vinci system is gaining popularity. This is owing to the articulating micro-robotic endo-wrist devices' capacity to conduct complex fine-motor movements in a small space.
The Da Vinci robot also has an extra third arm that allows for good retraction within the narrow pelvis, as well as a three-dimensional magnified image that allows visualization of the pre-sacral nerves associated with sexual function and hence their preservation.
The fundamental benefit of Robotic Ventral Mesh Rectopexy over perineal treatments is that it is a repair that addresses the root cause, which is a lack of adequate rectum support. It also prevents any perineal (vaginal or rectal) injuries, which means less pain and a lower chance of infection after surgery.
Conclusion
The use of robots in gastrointestinal surgery is still in its early stages. In Japan, public health insurance covers the expense of robotic surgery, as well as laparotomy and traditional laparoscopic surgery, for the majority of gastrointestinal diseases. As a result, for each patient with a gastrointestinal issue, surgical treatment options include laparotomy, traditional endoscopic surgery, and robotic surgery, with the type of operation chosen depending on the facilities and surgeons available. When considering public insurance, these surgical approaches must be separated to make the most of limited medical resources. For example, based on the patient's body type, BMI, specific anatomical features, and degree of disease progression, traditional endoscopic surgery should be chosen in cases where it can be done safely without a decrease in curability. In cases with a high degree of technical complexity, however, robotic surgery should be chosen to further ensure the safety and cure of the disease. Such individualized treatment could be a promising method of determining the best treatment.