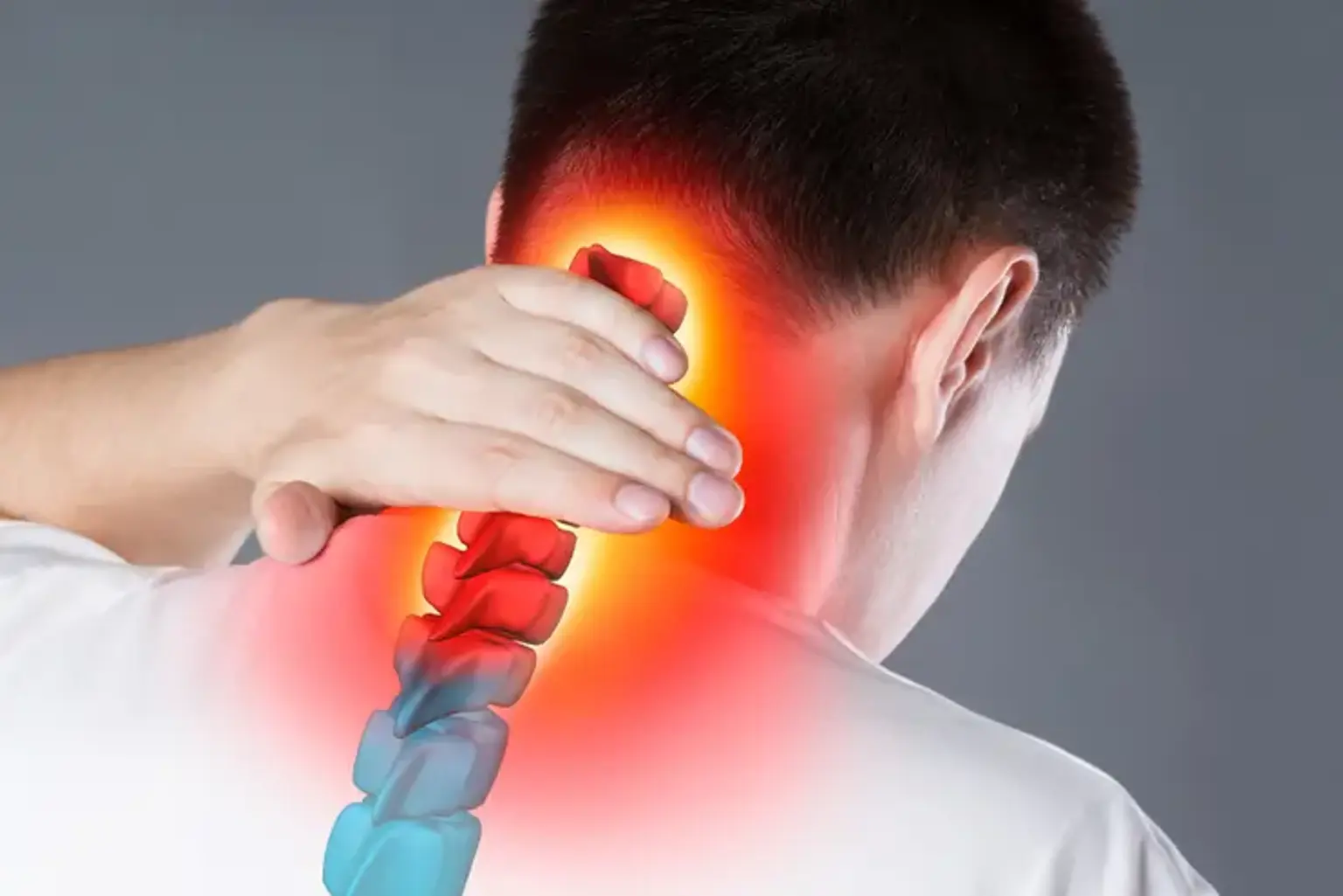
Cervical Herniated Nucleus
Cervical Herniated Disc
The vertebral column, often known as the spine, is made up of vertebrae and intervertebral discs. The cervical, thoracic, lumbar, and sacral areas are all included in this region, stretching from the skull’s base to the coccyx. The spine supports the body in several important ways, including providing structural support, safeguarding the spinal cord and branching spinal nerves, and allowing flexibility and mobility. The cartilaginous intervertebral discs between neighboring vertebrae act as shock-absorbing cushions to the axial loads of the body and support the spine.
Seven vertebral bodies make up the cervical spine, labeled C1 through C7, counting from the skull base to the thoracic spine. In contrast to the typical cervical vertebrae (C3 to C6) C1, C2, and C7 have different structural characteristics that set them apart from one another. The vertebral bodies, vertebral arches, and seven processes make up the anatomy of C3 to C6. The pedicles, bony processes that extend posteriorly from the vertebral body, and the lamina are the bone segments that make up the majority of the vertebral arch. The spinal canal, which houses the spinal cord, is surrounded by a ring formed by the pedicles and the lamina. Seven processes, including two superior and two inferior articular facets, one spinous process, and two transverse processes that permit the passage of the vertebral artery and vein, make up a normal vertebra.
The cervical area contains three unusual vertebrae. Due to its fusion with the C2 (axis) vertebrae, which serves as the atlas' pivot point, C1 (atlas), which articulates with the base of the skull, is unique in that it lacks a body. The presence of an odontoid process (dens), which rises from the superior part of the C2 vertebra's body and joins with the posterior surface of the anterior arch of C1, is the vertebra's most distinctive characteristic. In contrast to other cervical vertebrae, C7 differs from them in two key ways: first, the vertebral artery does not pass via its transverse foramina, and second, the spinous process is present, giving C7 the name vertebra prominens.