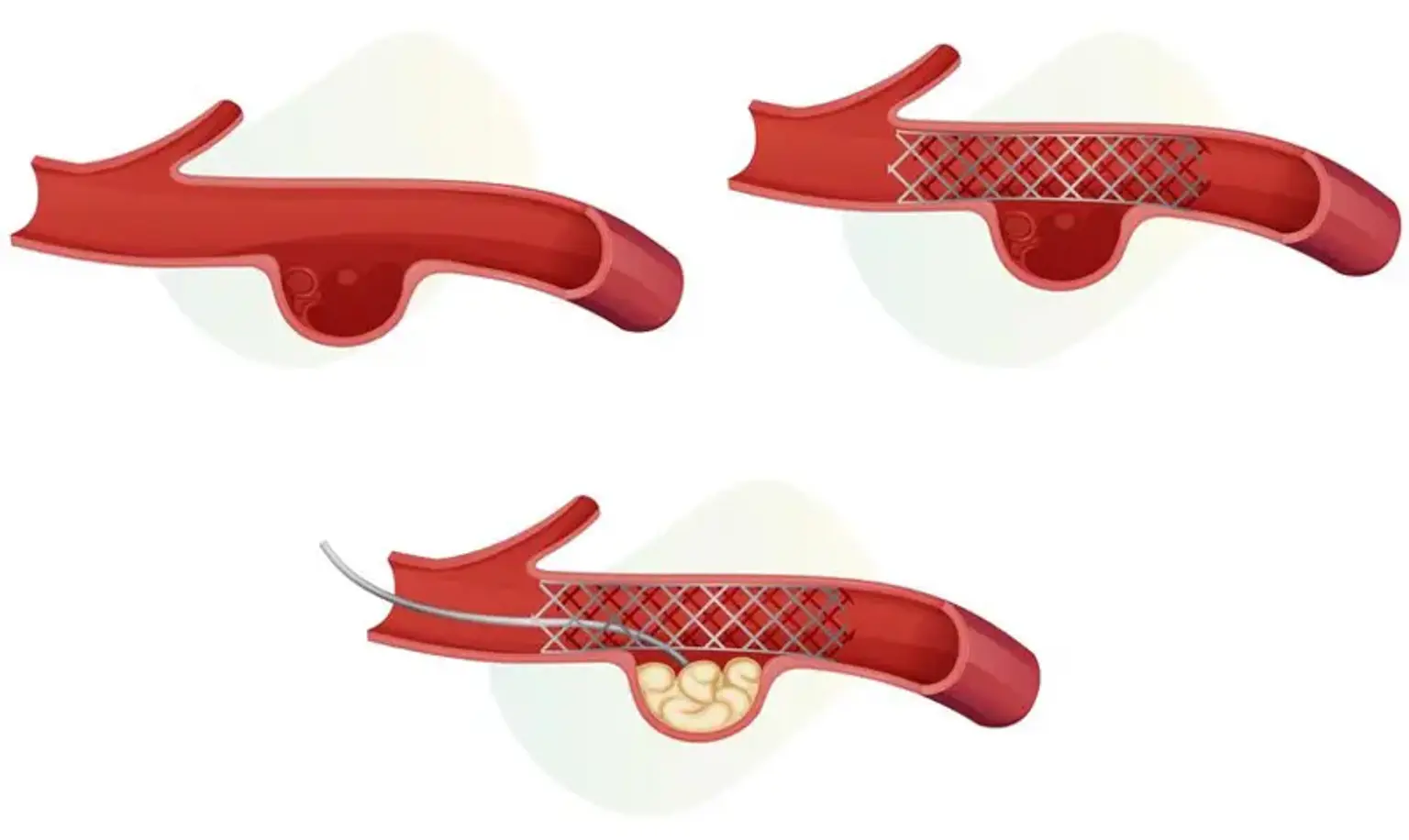
Endovascular Coiling
Overview
Endovascular coiling is a technique that is used to prevent blood flow into an aneurysm (a weakened area in the wall of an artery). Endovascular coiling is a relatively modern therapy for brain aneurysms, with patients having had it since 1991.
Endovascular coiling is a minimally invasive method that does not require a skull incision to cure a brain aneurysm. To access the aneurysm in the brain, a catheter is employed.
Endovascular coiling involves inserting a catheter via the groin into the artery containing the aneurysm. After that, platinum coils are released. The coils cause coagulation (embolization) of the aneurysm, preventing blood from entering it.
How Do I Get Ready for an Endovascular Coiling?
- Your healthcare professional will explain the process and give you the opportunity to ask questions.
- You will be asked to sign a consent form authorizing the treatment. If something is unclear, read the form carefully and ask questions.
- Inform your doctor if you have ever had an adverse reaction to a contrast dye or if you are sensitive to iodine.
- Inform your doctor if you are sensitive to or allergic to any medications, latex, tape, or anesthetic agents (local and general).
- Before the procedure, you must fast for a specific duration. Your doctor will advise you on how long you should fast, whether for a few hours or overnight.
- Inform your healthcare practitioner if you are pregnant or suspect you are pregnant.
- Inform your healthcare practitioner about all medications (prescription and over-the-counter) and herbal supplements you are using.
- If you have a history of bleeding problems or are using anticoagulant (blood-thinning) medications, aspirin, or other medications that alter blood clotting, inform your healthcare practitioner. You may need to discontinue these medications prior to the operation.
- Before the treatment, your healthcare professional may require a blood test to evaluate how long it takes your blood to clot. Other blood tests may also be performed.
- Your healthcare provider may request additional specific preparation based on your medical condition.
What Happens During an Endovascular Coiling?
You will need to stay in the hospital for a coiling procedure. Procedures may vary depending on your condition and your healthcare provider's practices.
Your procedure may be done by one or both of these specialists:
- Neurosurgeon. This healthcare provider specializes in surgery and treatment of the nervous system.
- Interventional radiologist. This healthcare provider specializes in diagnostic and treatment methods using radiology techniques.
You are sedated and under general anesthesia for the surgery. It may be done under local anaesthetic in some cases.
This is usually followed by a coiling procedure:
- You will be requested to remove any clothes, jewellery, hairpins, dentures, or other anything that might obstruct the process and will be provided a hospital gown to wear.
- Prior to the treatment, you will be given time to empty your bladder.
- On the X-ray table, you will be positioned on your back.
- In your hand or arm, an intravenous (IV) line will be inserted.
- An electrocardiogram (ECG) monitor will be attached to you to record the electrical activity of your heart. During the process, your vital signs (heart rate, blood pressure, and breathing rate) and neurological signals will be monitored.
- A catheter may be put into your bladder to empty urine.
- The radiologist or neurosurgeon will check your pulses below the groin location where the catheter will be put and mark them with a marker so that the circulation to the limb below the site may be monitored after the surgery.
- The skin over the injection site will be cleaned. A local anesthetic will be administered.
- A tiny incision will be made in the skin to expose the artery in the groin.
- A guide wire will be used to place a catheter into the artery in your groin. Fluoroscopy will be used to guide the catheter through the blood artery into the brain (a special type of X-ray, similar to an X-ray "movie").
- After guiding the catheter to the afflicted artery in the brain, contrast dye will be administered to make the aneurysm and surrounding blood arteries visible on X-ray.
- The aneurysm will be measured, as well as its form and other features.
- The primary catheter will then be replaced with a smaller catheter.
- Once the catheter has reached the aneurysm, the healthcare provider will insert the coil.
- When the coil has been fully placed into the aneurysm, it is disconnected from the catheter.
- The healthcare practitioner will place as many coils as necessary to completely close off the aneurysm. Inside the aneurysm, the coils will create a mesh-like structure.
- After the aneurysm has been "packed" with coils, additional X-ray images will be taken to make sure the aneurysm has been sealed off. The coil is left in place permanently in the aneurysm.
- Once the aneurysm has been sealed off, the catheter will be removed. After the insertion site stops bleeding, a dressing will be applied.
What Happens After an Endovascular Coiling?
- In the hospital
You may be transported to the recovery room or the intensive care unit (ICU) for observation following the surgery. If the coiling surgery was performed to treat a ruptured aneurysm, you would most likely be admitted to the intensive care unit for recovery and observation. If the coiling treatment was performed on an unruptured aneurysm and your condition is otherwise stable, you may be able to go home the next day or two.
You may be required to lie flat in bed for up to 12 hours following the treatment. Your vital signs, neurological signs, the insertion site, and circulation or sensations in the afflicted limb will all be monitored by a nurse.
You may be given pain medicine for pain or discomfort from the procedure or from having to lie flat and still for a prolonged period.
You may resume your usual diet after the procedure, unless your healthcare provider decides otherwise.
Once you have recovered, you may be able to go home, unless your healthcare provider decides otherwise. In some cases, after a procedure for a ruptured aneurysm, a transfer to a rehabilitation facility may be necessary to help continue recovery from damage that may have happened as a result of the ruptured aneurysm.
- At home
You may be advised not to do any strenuous activities. Your healthcare provider will instruct you about when you can return to work and resume normal activities. Tell your healthcare provider if you experience any of the following:
- Fever and/or chills.
- Increased pain, redness, swelling, or bleeding or other drainage from the insertion site.
- Coolness, numbness and/or tingling, or other changes in the affected extremity.
- Any changes in bodily functions or neurological changes, such as extreme headache, seizure, or loss of consciousness.
A cerebral angiography is usually performed following the treatment to ensure that the coiling is operating properly. The first angiography may be performed around one month following the operation. Other imaging techniques, including as MRI or MRA, may be performed at intervals chosen by your healthcare practitioner based on your condition and the outcomes of prior post-coiling imaging treatments.
Other specific directions regarding what to do following endovascular coiling may be given to you by your healthcare practitioner.
Alternatives to Endovascular Coiling
- Active observation
If the risk of rupture is low, an active surveillance approach is usually indicated.
This means you won't have surgery right away, but you will have frequent check-ups so your aneurysm can be closely monitored.
You may also be prescribed blood pressure medicine.
Your doctor will discuss lifestyle modifications, such as decreasing weight and consuming less saturated fat, that can help reduce the chance of a rupture.
- Neurosurgical clipping
Neurosurgical clipping is performed under general anaesthesia, so you will be unconscious during the procedure.
A thin flap of bone is taken from your head, or occasionally just above your brow, to provide the surgeon access to your brain.
After locating the aneurysm, the neurosurgeon will seal it shut with a small metal clip that remains permanently clamped on the aneurysm. The scalp is stitched together once the bone flap has been restored.
The blood vessel lining will repair along the clip placement line over time, permanently closing the aneurysm and preventing it from expanding or rupturing in the future.
Clipping the artery where the aneurysm is developed, rather than the aneurysm itself, is rarely essential. This is usually only carried out if the aneurysm is particularly large or complex.
When this is required, it is frequently paired with a technique known as a bypass. The blood flow is rerouted around the clamped area by utilizing a blood artery taken from another part of the body, commonly the leg.
Endovascular Coiling Vs Clipping
- Clipping Procedure
Aneurysm clipping is a surgical operation in which the surgeon enters the blood artery directly via a craniotomy and then inserts a metal clip at the base of the aneurysm, cutting it off from the blood supply. This decreases the chance of future rupture by preventing blood from flowing into the weaker pouched region. Some surgeons will do a microcraniotomy or access the blood supply through the brow, but the usual treatment is a craniotomy and removal of part of the skull.
Advantages:
- Clipping Is An Established and Safe Procedure
The clipping operation has been used to treat aneurysms in the brain for decades, thus its safety and efficacy have been well established. Clipping has been practiced long enough that research on outcomes in a significant number of patients have been performed, and the operation has been fine-tuned for even better results. - Clipping Can Treat Most Aneurysms
Clipping surgery can be performed on most types of aneurysms, even those that have already ruptured. The clipping procedure can also be done on aneurysms that are considered difficult to treat, such as those with a wide neck at the base. - Clipping Lowers the Risk of Recurrence
Because well-clipped aneurysms have a very low risk of recurrence, the clipping treatment effectively resolves the aneurysm for many individuals. This means that for many patients, particularly younger ones, the risk of an aneurysm recurrence is quite low.
Disadvantages:
- Clipping Is An Invasive Procedure
Although aneurysm clipping has been proved to be a safe and successful method of treatment, it is an invasive surgery that requires opening the skull. In order to reach the aneurysm, neurosurgeons must conduct a craniotomy to remove a part of the skull and cut into brain regions. - Clipping Requires General Anesthesia
Because clipping is an intrusive process, it needs general anesthesia. General anesthesia is hazardous, especially for elderly people and those with chronic medical issues. During their recovery, these individuals will need to be closely observed. - Clipping Requires a Longer Recovery Time
Because clipping is an invasive procedure, recovery time is usually prolonged. Without difficulties, healing from a clipping treatment performed on an unruptured aneurysm can take two to five days in the hospital and 3-6 weeks at home. Recovery might take much longer if the treatment was performed on a ruptured aneurysm.
- Coiling Procedure
Coiling is an endovascular procedure, which means the surgeon accesses the aneurysm through the vascular system.
Advantages:
- Coiling Is Less Invasive Than Clipping
Aneurysm coiling requires only a single incision in the leg to reach the major femoral artery, eliminating the need to expose the skull or brain. This incision usually heals fast with little scars. - Coiling Is Safer for At-Risk Patients
Because clipping surgery is invasive, it may not be recommended for elderly individuals or those with specific health issues. Coiling's less invasive nature may make it a safer choice for treating aneurysms in high-risk individuals. - Coiling Has a Shorter Recovery Time Than Clipping
Patients often recover faster after coiling since it is significantly less invasive than clipping. Patients who have no issues often spend a day or two in the hospital and may resume most routine activities within a week.
Disadvantages:
- Some Aneurysms Cannot Be Treated With Coiling
Clipping can cure aneurysms of many shapes and sizes, while coiling is not suited for certain, such as aneurysms with a very wide neck or particular forms. If an aneurysm has already ruptured, coiling may not be an option. - Coiling Requires General Anesthesia
Although less invasive than clipping, coiling is still a surgical procedure that requires general anesthesia, with the usual risks and concerns. - Coiling May Require Blood Thinning Therapy
Patients must take one or more anticoagulant, or blood-thinning, drugs both before and after coiling to limit the risk of serious clotting. Depending on the conditions, patients may need to take these drugs for an extended length of time following coiling. - Imaging Tools Can Be Risky
During a coiling procedure, surgeons use tools, including x-ray imaging and dyes, to guide the placement of the coils. That exposes a patient to risks from radiation for the duration of the procedure, or to allergic reactions to injected dyes. - Coiling Is Relatively New
Aneurysm coiling was first used in 1991. While this relatively new technology for treating aneurysms has been shown to be safe and effective, fewer studies have been done on its long-term outcomes and rates of completely resolving aneurysms.
What are the Risks of Endovascular Coiling?
If you are pregnant or suspect that you are pregnant, you should notify your healthcare professional.
There is a chance of an adverse reaction to the dye used to see the aneurysm on X-ray. Individuals who are allergic or sensitive to medications, contrast dye, or iodine should notify the radiologist or technician. People who have renal failure or other kidney issues should notify the radiologist.
People who use anticoagulant (blood-thinning) medications, such as aspirin, warfarin, clopidogrel, or others, should notify their doctors before the surgery. These medications may be discontinued for one or more days prior to the surgery.
Because the procedure involves the blood vessels and blood flow of the brain, there is a risk for complications involving the brain. These complications may include:
- Loss of consciousness.
- Stroke or transient ischemic attack (TIA, a temporary stroke-like condition).
- Paralysis of one half of the body.
- Blood clot.
- Bleeding.
- An area of swelling caused by a collection of blood (hematoma).
- Loss of the ability or speak or the ability to understand speech (aphasia).
- Infection.
- Rupture of unruptured aneurysm.
- Higher chance of an aneurysm recurring.
- There may be other risks depending on your specific medical condition. Discuss any concerns with your healthcare provider before the procedure.
Conclusion
Endovascular coiling, also known as endovascular embolization, is a technique used by doctors to stop blood flow into an aneurysm. An aneurysm is a weak spot in the arterial wall. Aneurysm rupture can result in life-threatening bleeding and brain injury. Preventing blood flow into an aneurysm aids in its prevention from rupturing.
Endovascular coiling is performed with a catheter, which is a long, thin tube placed into a groin artery. The catheter is inserted into the damaged cerebral artery, where the coil is inserted. X-rays aid in the placement of the catheter in the artery. The coils are constructed of soft platinum metal and are spring-shaped. These coils are extremely tiny and thin, ranging in size from roughly twice the thickness of a human hair to less than the breadth of one hair.
Coiling is also used by doctors to treat a disorder known as arteriovenous malformation, or AVM. AVMs are improper connections between arteries and veins. It can occur in the brain, spinal cord, or anywhere else in the body.