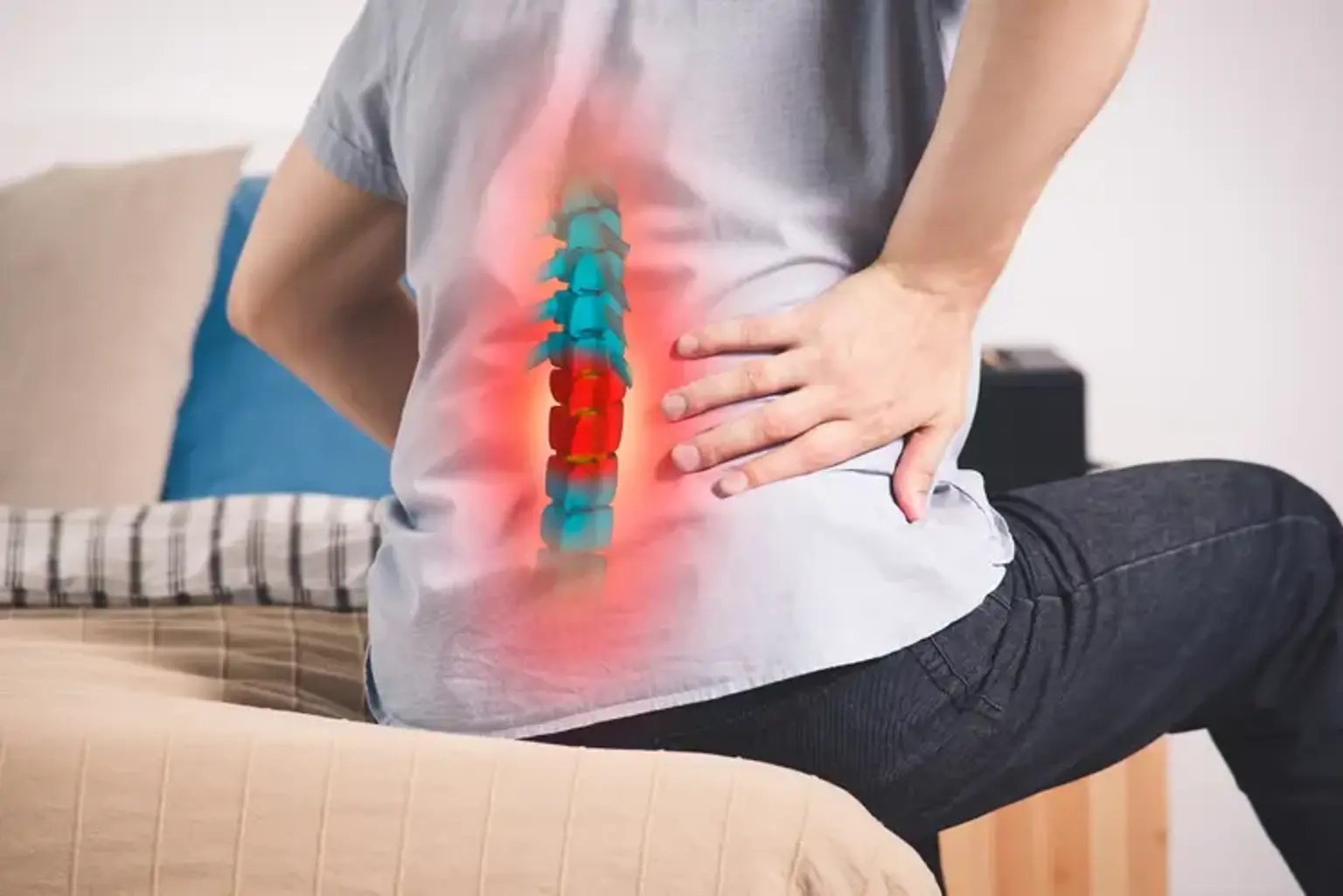
Medial Branch Nerve Blocks
The tiny nerves known as medial branch nerves are what allow you to experience pain in facet joints. The facet joints are tiny joints that connect each vertebra at the back of the spine. There are four facet joints on each vertebra, two on the upper or superior surface and two on the lower or inferior surface. The facet joints control how far your neck and back can be bent or twisted.
The neck and the mid or low tiny back muscles are under the control of the facet joint medial nerves. Your arms and legs don't have any muscles or sensations controlled by them. A medial branch nerve block made of steroids and anesthetic drugs might temporarily stop the pain signal originating from a certain facet joint if it has been determined that your discomfort originates from the facet nerves of certain facet joints.