Introduction
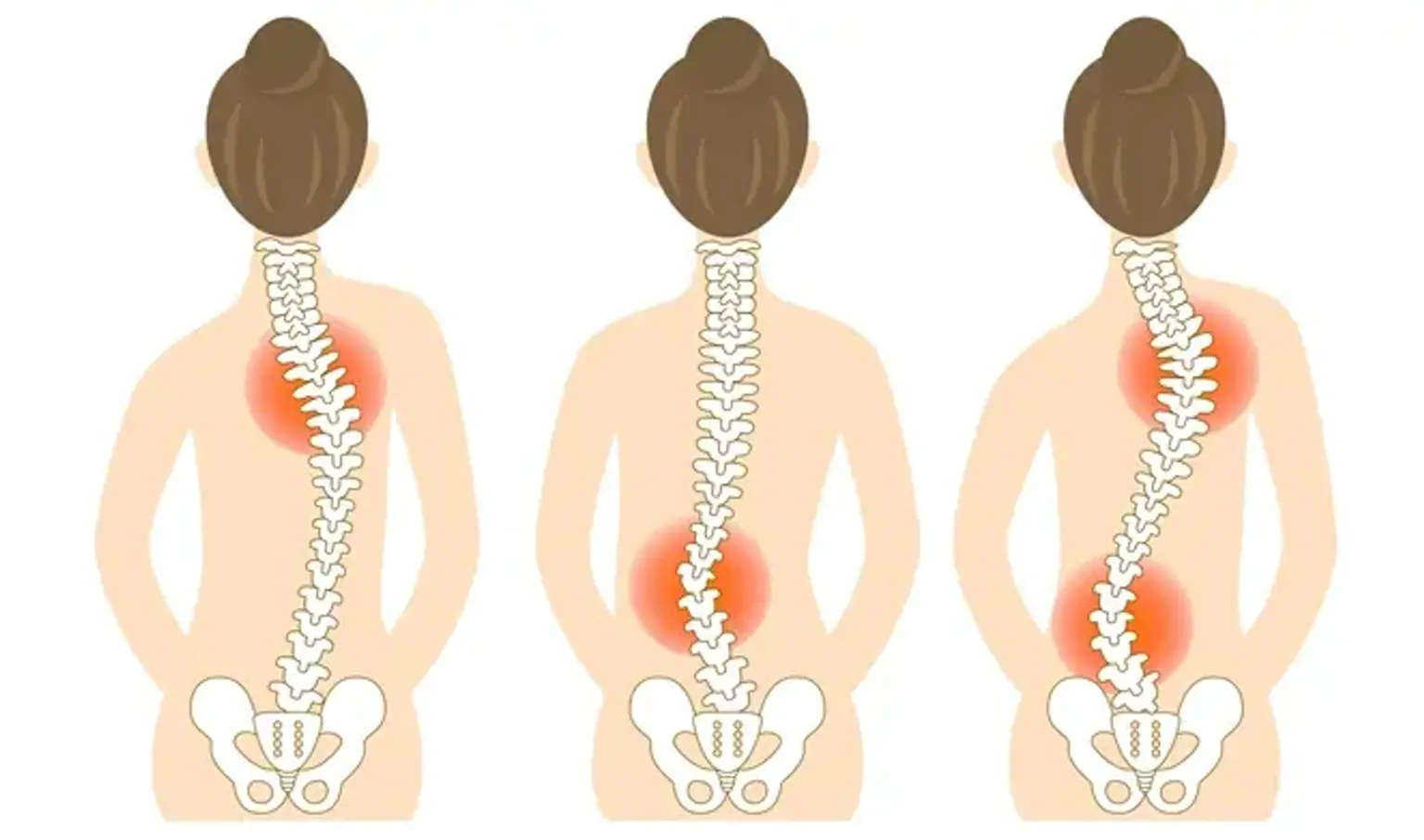
Scoliosis is a condition where the spine curves abnormally, often resembling an "S" or "C" shape. It affects people of all ages but is most commonly diagnosed in children and adolescents. Spinal deformities like scoliosis, kyphosis (forward curvature), and lordosis (excessive inward curve) can lead to discomfort, pain, and even functional impairments if left untreated.
While mild scoliosis may not be immediately noticeable, severe cases can cause significant postural issues and, in some cases, lead to difficulties with breathing or mobility. Early diagnosis and treatment are crucial to prevent progression, particularly in growing children.
Understanding the Different Types of Scoliosis
There are several types of scoliosis, each with distinct causes:
Idiopathic Scoliosis: The most common type, especially among adolescents. Its cause is unknown, though genetics may play a role.
Congenital Scoliosis: Present from birth due to abnormal spinal development.
Neuromuscular Scoliosis: Associated with conditions like cerebral palsy or muscular dystrophy, affecting muscle control and spinal stability.
Degenerative Scoliosis: Develops in adults due to age-related changes in the spine, such as disc degeneration or arthritis.
Additionally, scoliosis can be functional (temporary and caused by other conditions like leg length discrepancies) or structural (permanent changes to the spine itself).
Causes and Risk Factors of Scoliosis
The exact cause of scoliosis is still largely unknown, but several factors contribute to its development:
Genetics: Family history can increase the likelihood of developing scoliosis, especially in idiopathic cases.
Age and Gender: Adolescents, particularly girls, are more likely to develop scoliosis, with symptoms typically appearing between ages 10 and 18.
Neurological and Muscular Conditions: Conditions like cerebral palsy and muscular dystrophy can lead to neuromuscular scoliosis due to weakened muscles around the spine.
Environmental Factors: While poor posture is often blamed, there is limited evidence that it causes scoliosis. However, lifestyle factors like heavy backpacks in children may contribute to discomfort.
Symptoms and Signs of Scoliosis
Scoliosis symptoms vary depending on the severity and type of curvature:
Physical Signs: Uneven shoulders, hips, or rib cage. In severe cases, one side of the back may appear more prominent.
Pain and Discomfort: Not everyone with scoliosis experiences pain, but some individuals report chronic back pain, especially in adults with degenerative scoliosis.
Postural Changes: A noticeable shift in posture, where the body leans to one side, may occur. This can affect balance and movement.
As scoliosis progresses, it may lead to difficulty breathing if the curvature impacts lung capacity. Early signs should be checked by a healthcare provider, particularly in growing children.
How Scoliosis is Diagnosed
Diagnosing scoliosis usually involves a combination of a physical exam and imaging tests:
Physical Examination: A doctor will look for visible signs such as uneven shoulders or hips. They may ask the patient to bend forward to observe any curvature in the spine.
X-rays: The most common diagnostic tool, X-rays help determine the degree of curvature and track changes over time.
MRI and CT Scans: These imaging tests are used for detailed views of the spine when there is concern about nerve involvement or other complications.
Scoliometer: A device used to measure the angle of the spine's curvature.
If scoliosis is suspected, a thorough evaluation will help determine the most effective treatment plan based on the type and severity of the condition.
Treatment Options for Scoliosis
Treatment for scoliosis depends on the severity of the curvature and the age of the patient:
Non-Surgical Treatments:
Bracing: Often used for adolescents with moderate scoliosis to prevent further curvature. Braces don't correct the curve but can stop it from worsening.
Physical Therapy: Focuses on strengthening muscles and improving posture. While it can't straighten the spine, it helps alleviate discomfort.
Observation: For mild cases or in growing children, doctors may recommend monitoring the curve to see if it worsens.
Surgical Treatments:
Spinal Fusion: A procedure where two or more vertebrae are fused together to stabilize the spine.
Rod Implantation: Metal rods may be inserted to straighten the spine.
Minimally Invasive Surgery: Uses smaller incisions, offering less pain and faster recovery.
The choice of treatment depends on the curvature angle, symptoms, and patient health.
Minimally Invasive Surgery for Scoliosis
Minimally invasive surgery (MIS) is becoming a popular option for scoliosis correction:
What is MIS?: This approach involves smaller incisions, often using specialized instruments and sometimes robotic assistance, to straighten the spine.
Benefits: MIS reduces blood loss, minimizes scarring, and speeds up recovery time compared to traditional surgery.
Who is a Candidate?: MIS is best suited for patients with less severe curves and those who have not had previous spinal surgery.
Outcomes: While the effectiveness of MIS can be just as successful as traditional surgery, the approach offers quicker recovery and less pain post-operation.
Spinal Fusion Surgery for Scoliosis Correction
Spinal fusion is the most common surgical treatment for severe scoliosis:
Procedure: The surgeon uses metal rods, screws, and sometimes bone grafts to straighten and stabilize the spine. The bones are then fused together to prevent further curvature.
Benefits: This surgery can greatly reduce pain, improve posture, and stop the curve from worsening. It’s especially effective in severe cases.
Risks: Like any surgery, spinal fusion carries risks, including infection, nerve damage, and complications with the hardware.
Recovery: Recovery takes time—patients typically stay in the hospital for 4–7 days and can expect to resume normal activities in 6–12 months, depending on individual healing.
The Role of Bracing in Scoliosis Treatment
Bracing is often recommended for children and adolescents whose scoliosis curves are moderate and still developing:
When Is Bracing Used?: Braces are most effective for adolescents whose bones are still growing. The goal is to prevent further progression of the curve.
Types of Braces: Common options include the Boston Brace (a custom-molded plastic brace), the TLSO (Thoraco-Lumbo-Sacral Orthosis), and the Charleston Bending Brace (worn at night for more severe curves).
Effectiveness: Bracing doesn’t cure scoliosis but can halt or slow curve progression, particularly if worn consistently.
Challenges: The psychological and emotional impact of wearing a brace can be significant, especially in teenagers. Some may feel self-conscious or uncomfortable.
Alternative and Complementary Treatments for Scoliosis
While surgery and bracing are the primary treatments, some patients turn to alternative therapies:
Chiropractic Care: Chiropractors may offer spinal adjustments aimed at improving posture and reducing pain, but it does not correct the curvature.
Physical Therapy: Exercises can help strengthen muscles around the spine, alleviate pain, and improve flexibility. Specific techniques like the Schroth Method are designed to improve posture and manage scoliosis.
Acupuncture and Massage Therapy: These therapies may help with pain management and overall relaxation, but there’s no evidence they can correct scoliosis.
Nutritional Support: Proper nutrition, including calcium and vitamin D, is essential for bone health and may support overall spinal health, particularly after surgery.
The Global Appeal of Scoliosis Treatment
Scoliosis treatment has become a global concern, with different countries offering varying levels of care:
Developed Countries: In countries like the U.S., Germany, and Japan, advanced surgical techniques, including robotic-assisted surgeries and minimally invasive procedures, are widely available.
Challenges in Developing Regions: Limited access to healthcare and surgical expertise makes scoliosis treatment a challenge in low-resource settings. Many patients don’t receive timely diagnoses or the care they need.
Medical Tourism: Some patients travel abroad to access high-quality scoliosis surgery at lower costs, especially in countries like India, Mexico, and Thailand.
International Collaboration: Organizations and medical professionals worldwide are working together to improve treatments and provide support for scoliosis patients in underserved areas.
Expected Results After Scoliosis Treatment
After receiving treatment for scoliosis, patients can typically expect the following outcomes:
Post-Surgery Results: The primary goal of surgery, such as spinal fusion, is to reduce the curvature and prevent it from worsening. Patients often experience improved posture, reduced pain, and better spinal alignment.
Long-Term Benefits: Correcting scoliosis can significantly improve quality of life. Many patients report enhanced mobility and decreased discomfort, allowing them to resume normal activities.
Psychological Impact: Beyond physical benefits, successful treatment can boost self-esteem and body image, especially for adolescents who may feel self-conscious about their appearance.
Follow-Up Care: Ongoing monitoring through X-rays ensures that the spine remains stable and that any potential complications are detected early. Physical therapy may continue to strengthen the back and maintain flexibility.
The Recovery Process After Scoliosis Surgery
Recovery after scoliosis surgery is a gradual process, and how quickly a patient heals can depend on factors like the type of surgery and their overall health:
Initial Recovery: After surgery, patients typically stay in the hospital for 4–7 days. The first few days will focus on pain management and helping the patient regain mobility.
Physical Therapy: Once the initial healing phase is over, physical therapy plays an essential role in recovery. It helps patients regain strength, flexibility, and normal movement.
Time to Full Recovery: It can take anywhere from 6 to 12 months to fully recover after spinal fusion surgery, with most patients resuming regular activities in about a year. During recovery, activities that stress the spine (like heavy lifting) should be avoided.
Follow-Up Care: Regular follow-up visits are crucial to monitor the progress of the spine and ensure the fusion is healing correctly. X-rays will often be used to check the alignment.
Lifestyle Adjustments After Scoliosis Treatment
After scoliosis treatment, particularly surgery, certain lifestyle adjustments are necessary to maintain spinal health and prevent future issues:
Post-Surgery Restrictions: Initially, patients should avoid activities that put strain on the spine, such as high-impact sports or heavy lifting. It's essential to follow the doctor’s recommendations for physical activity.
Regular Exercise: Once cleared by a physician, regular low-impact exercises (e.g., walking, swimming) can help maintain overall health and strengthen muscles around the spine.
Healthy Posture: Maintaining proper posture is vital for spinal health. Standing and sitting with a straight back can help reduce strain on the spine.
Weight Management: Maintaining a healthy weight is important to reduce the load on the spine, particularly for patients with degenerative scoliosis in adulthood.
Long-Term Monitoring and Maintenance
Even after successful treatment, long-term monitoring of scoliosis is essential to ensure continued spinal health:
X-Rays and Regular Checkups: Patients may need periodic X-rays to track the alignment of the spine, especially in younger patients who are still growing or those who had surgery.
Physical Therapy Maintenance: Even after initial recovery, continuing physical therapy or at-home exercises can maintain flexibility and muscle strength, which are crucial to supporting the spine.
Surgical Follow-Ups: For those who had surgery, it's vital to stay in touch with the surgical team for any necessary adjustments or to address concerns like hardware failure (though this is rare).
Frequently Asked Questions about Scoliosis Treatment
Here are some common questions people ask about scoliosis treatment:
1. Can scoliosis be prevented?
While there's no surefire way to prevent scoliosis, early detection through regular check-ups can help catch it before it worsens.
2. Is scoliosis treatment painful?
Treatment options like bracing and physical therapy generally cause minimal discomfort. However, surgery involves a recovery period with pain management.
3. Will scoliosis surgery leave a visible scar?
Surgery involves an incision along the back, but modern surgical techniques, including minimally invasive options, help reduce scarring.
4. Can I still live an active life after scoliosis surgery?
Yes! After the recovery period, most patients can return to normal activities, though high-impact sports may be restricted.
5. How successful is scoliosis surgery?
Scoliosis surgery has a high success rate, with most patients experiencing significant improvements in posture, pain reduction, and quality of life.
6. Are there non-surgical treatments for scoliosis?
es, treatments like bracing and physical therapy can help manage mild to moderate scoliosis, especially for children and adolescents.
The Psychological Impact of Scoliosis
Scoliosis can have significant psychological effects, particularly for adolescents and young adults:
Self-Esteem and Body Image: The visible deformity from scoliosis may affect how individuals view their appearance, leading to feelings of insecurity or self-consciousness. This is especially true for teenagers who are in a critical phase of identity development.
Emotional Wellbeing: Chronic pain and limited mobility can contribute to anxiety and depression. It's important for patients to have emotional support from family, friends, and mental health professionals during their treatment journey.
Social Impact: Patients may avoid social situations, particularly in young adults, due to the stigma of wearing a brace or having visible spinal deformities. Support groups or counseling can help address these challenges.
Treatment Outcomes: Positive changes in appearance after successful treatment can significantly improve self-esteem and overall emotional health.
The Cost of Scoliosis Treatment
The cost of scoliosis treatment can vary widely based on the severity of the condition, the treatment method chosen, and geographical location:
Non-Surgical Treatments: Bracing costs can range from $2,000 to $7,000, depending on the type of brace and the duration of use. Physical therapy may cost several hundred dollars per session, especially if long-term treatment is required.
Surgical Costs: The cost of scoliosis surgery, including hospitalization, anesthesia, and follow-up care, can range from $20,000 to $100,000 or more, depending on the complexity of the surgery and where it’s performed.
Insurance Coverage: Many health insurance plans cover scoliosis treatments, but out-of-pocket costs can still be significant. Patients are encouraged to check with their insurance provider to understand coverage details.
Financial Assistance: For patients without insurance or those facing high costs, some hospitals and organizations offer financial assistance programs.
Advancements in Scoliosis Treatment
The field of scoliosis treatment has seen significant advancements in recent years:
Robotic-Assisted Surgery: Robotic systems are now used to help surgeons perform precise, minimally invasive scoliosis surgery, which reduces recovery time and improves outcomes.
3D Imaging Technology: Advances in 3D imaging allow surgeons to plan surgeries with higher accuracy, resulting in better alignment and fewer complications.
Spinal Growth Modulation: In younger patients, new technologies are being used to guide spinal growth and reduce the need for invasive surgery. This includes growing rods or adjustable implants that help control the curvature as the child grows.
Personalized Bracing: Custom-fitted braces, made using 3D scans, are now more effective and comfortable than ever, improving patient adherence and outcomes.
These innovations offer hope for less invasive treatments and better results in managing scoliosis, particularly in younger patients.
Conclusion
The future of scoliosis treatment looks promising with ongoing advancements in technology and care:
Less Invasive Techniques: As minimally invasive surgery and robotic assistance become more refined, patients can expect quicker recovery times, fewer complications, and more accurate results.
Personalized Care: The rise of 3D imaging, personalized braces, and individualized treatment plans will help tailor care to each patient’s unique needs, improving outcomes.
Preventive Measures: Ongoing research may uncover better methods for preventing scoliosis or halting its progression before it requires surgery.
Global Access to Treatment: As medical tourism continues to grow and healthcare access improves globally, more patients will have the chance to receive high-quality scoliosis care, regardless of their location.
In conclusion, with early detection, personalized treatment options, and emerging technologies, scoliosis can be managed effectively, helping patients lead healthier, more active lives.