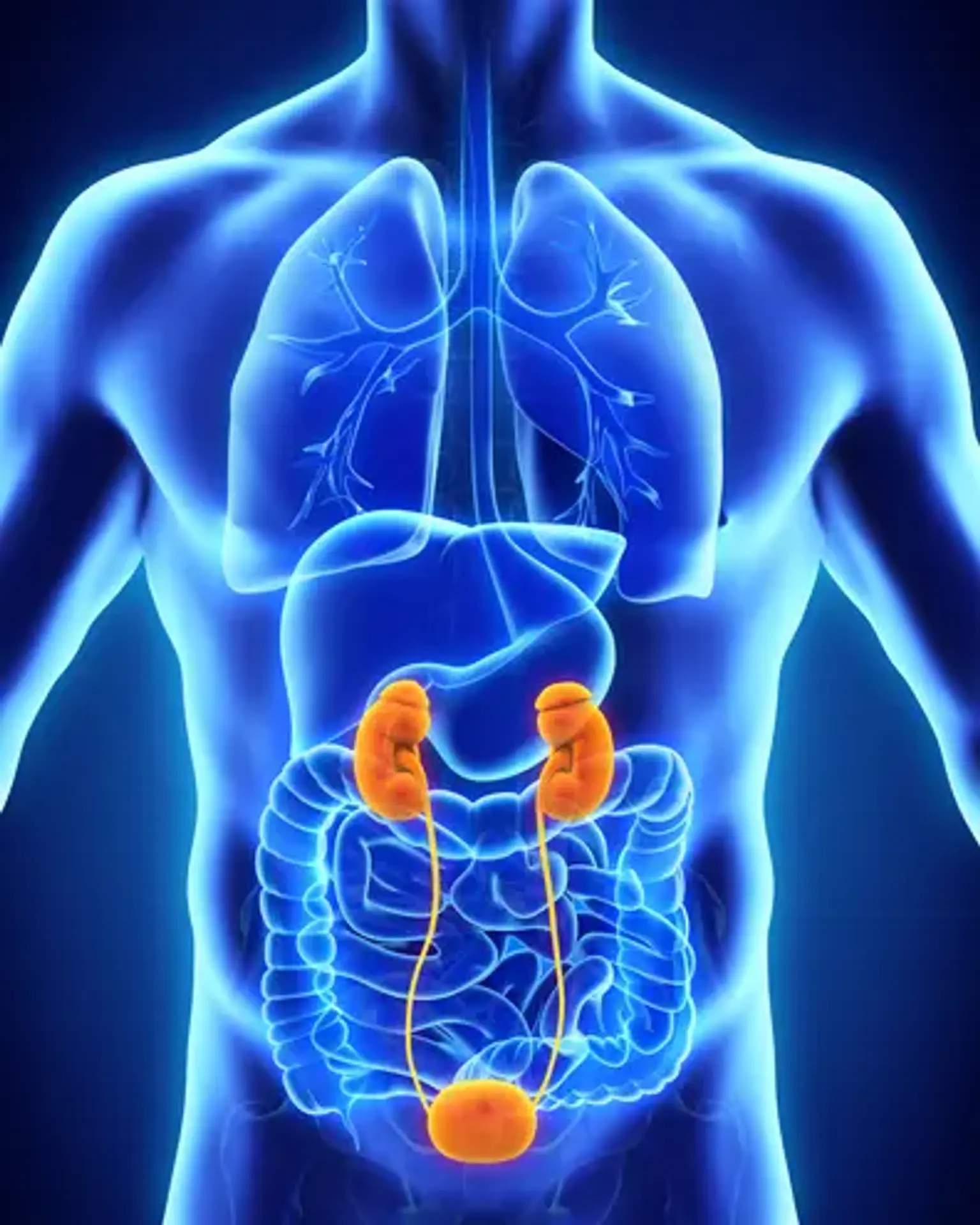
Ureteral Diseases
Overview
Urine is produced by your kidneys by filtering wastes and excess water from your blood. Urine flows from the kidneys to the bladder via two narrow tubes known as ureters. Ureters range in length from 8 to 10 inches. To drive urine down and away from the kidneys, muscles in the ureter walls tense and release. Every 10 to 15 seconds, little volumes of pee flow from the ureters into the bladder. The ureters can become clogged or damaged at times. This can obstruct urine passage to the bladder.