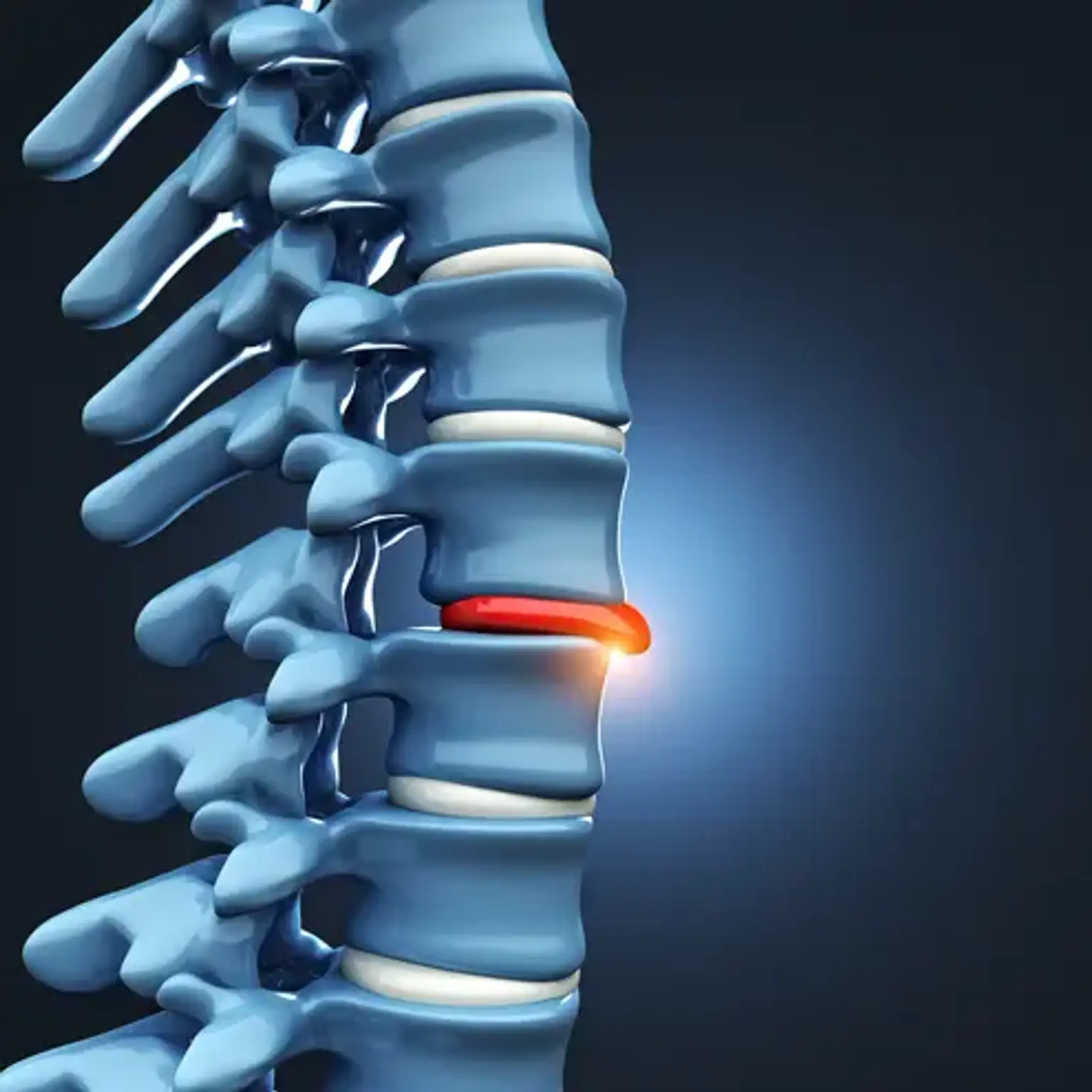
Lumbar Herniated Disc
Overview
Low back pain is a common complaint, affecting around 80% of the population at some point in their lives. The most prevalent cause of low back pain is intervertebral degeneration, which leads to lumbar disc herniation and degenerative disc disease.