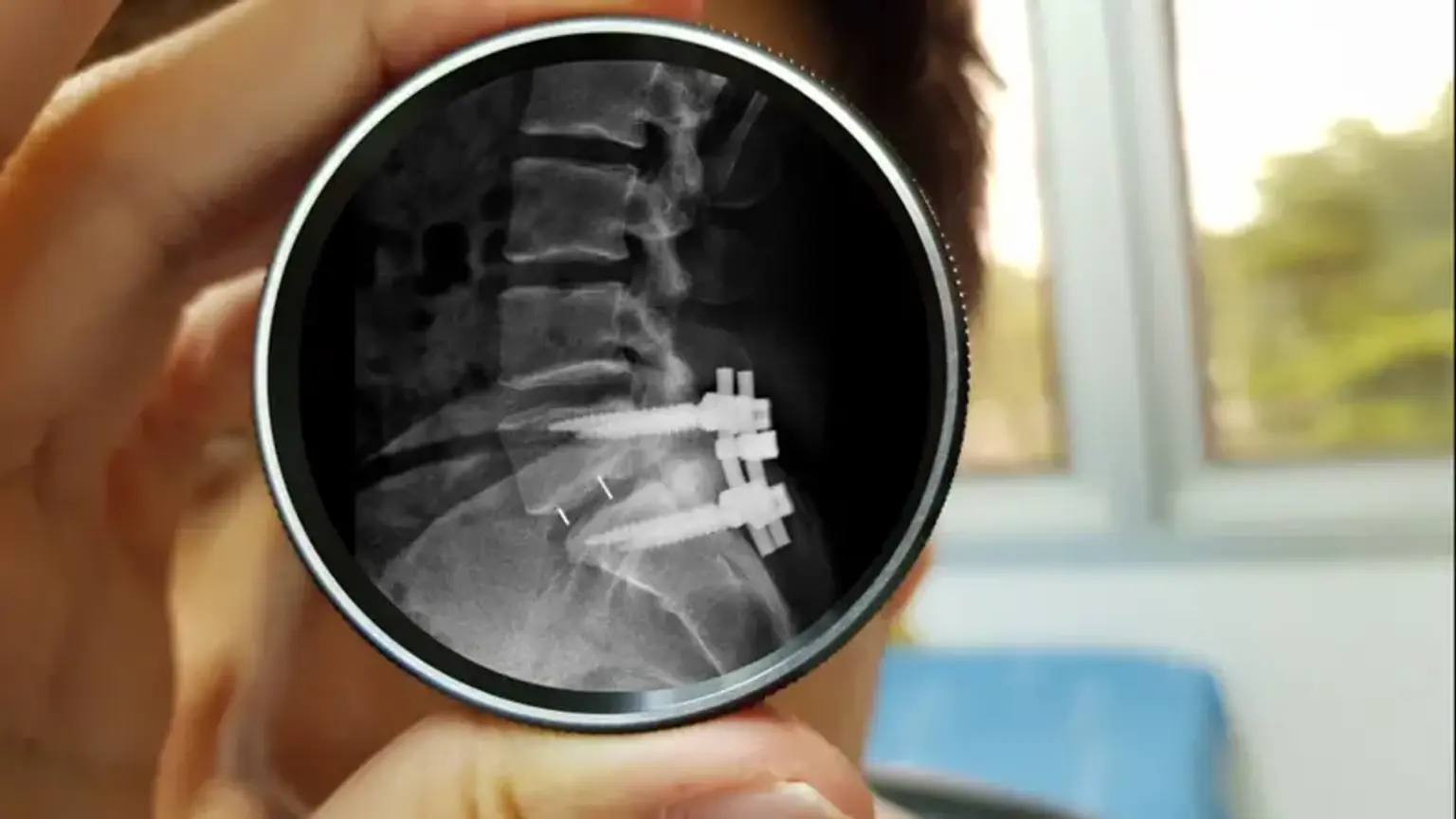
mini TLIF + PPF
There might be substantial discomfort in the legs and lower back when a patient has degenerative disc disease, recurrent disc herniation, or spondylolisthesis. By stabilizing the spinal vertebrae and the disc between them, fusing two or more discs together can help relieve discomfort. If at all possible, surgeons prefer to fuse the spine using the transforaminal lumbar interbody fusion (TLIF) procedure. They feel that TLIF produces outstanding results in the right patient population.
What is Mini TLIF with PPF
The posterior and transverse portions of the spinal column are fused via a procedure known as transforaminal interbody fusion, or TLIF. Understanding this method requires some fundamental vocabulary. The term transforaminal refers to passage through or across the foramina. The foramina are holes or openings in the bone that allow membrane structures to be inserted. The term interbody refers to the tissue that exists between two spinal sections and maintains disc height and spacing. Fusion is a medical term that refers to the surgical union or connection of bones for the purpose of healing.