Introduction
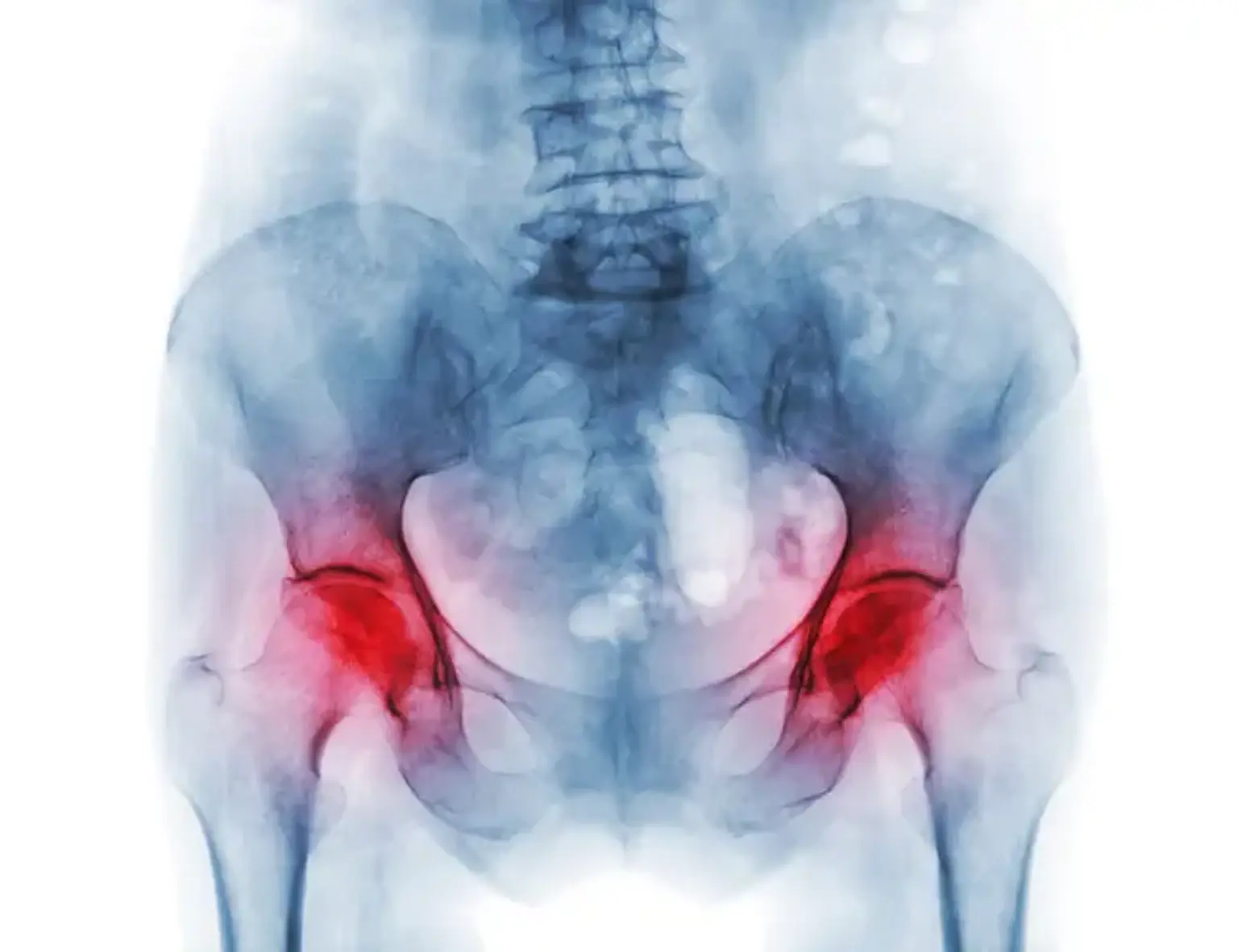
Avascular necrosis (AVN), also known as osteonecrosis, is a condition where bone tissue dies due to a lack of blood flow. This leads to the collapse of the bone and, if left untreated, can cause severe joint damage. AVN often affects the hip joint but can occur in other areas like the knee, shoulder, and ankle.
Early diagnosis and treatment are essential for preventing long-term disability and preserving joint function.
Surgical Treatment for Avascular Necrosis
When non-surgical treatments fail, or if the condition reaches an advanced stage, surgical options may be required:
Core Decompression: Although it is also a non-invasive treatment, in more severe cases, core decompression can be performed in combination with bone grafting or other surgical techniques to prevent further bone collapse.
Bone Grafting: Involves taking healthy bone tissue (either from another part of the body or from a donor) and placing it into the affected area. This can help promote healing and provide additional strength to the bone.
Osteotomy: In cases where the bone is deformed, osteotomy involves cutting and repositioning the bone to relieve pressure on the joint.
Joint Replacement Surgery: For advanced stages of AVN, especially in the hip or knee, joint replacement surgery is the most effective treatment. The damaged joint is replaced with a prosthetic, improving function and relieving pain.
Recovery after surgery depends on the extent of the procedure, with joint replacement generally requiring several months for rehabilitation and physical therapy.
Understanding the Causes of Avascular Necrosis
Avascular necrosis occurs when the blood supply to the bone is interrupted, causing bone cells to die. The most common causes include:
Trauma or Injury: Fractures or dislocations can disrupt blood flow to the bone.
Steroid Use: Long-term use of corticosteroids is a leading cause of AVN.
Excessive Alcohol Consumption: Alcohol can affect bone health by reducing blood flow.
Medical Conditions: Diseases like sickle cell anemia, lupus, and diabetes increase the risk of AVN.
Blood Disorders: Conditions that affect blood clotting or circulation can lead to reduced blood flow to the bone.
The Role of Joint Replacement Surgery in Avascular Necrosis
When AVN causes significant damage to the joint and other treatments are not sufficient, joint replacement surgery may be necessary. This is especially common in hip and knee avascular necrosis. Here’s what to expect:
Hip Replacement: The femoral head (top of the thigh bone) is replaced with a prosthetic. This is the most common surgical solution for severe hip AVN.
Knee Replacement: For patients with AVN in the knee, a total or partial knee replacement can restore joint function and alleviate pain.
Recovery Process: After joint replacement surgery, patients will go through a rehabilitation process to regain strength and mobility. Most people experience significant pain relief and improved function after recovery.
Long-Term Outcomes: Joint replacements typically last 15-20 years, depending on the patient's activity level and the type of prosthetic used. Regular follow-up care is essential to monitor for wear or complications.
While joint replacement surgery is highly effective in restoring function, it is typically reserved for cases where other treatments have failed.
Staging of Avascular Necrosis
Avascular necrosis progresses in stages, with each stage influencing the treatment options and prognosis. The stages are generally classified as follows:
Stage 1: Early AVN with no visible changes on X-ray, but MRI shows bone damage. This stage is the most treatable, and non-surgical treatments are often effective.
Stage 2: Mild bone collapse is visible, but the joint is still functional. Non-surgical treatments, including core decompression, may be recommended.
Stage 3: More severe bone collapse, with joint pain and loss of function. Surgical options, such as bone grafting or osteotomy, become necessary.
Stage 4: Severe joint damage with complete collapse of the bone. At this stage, joint replacement surgery, such as hip or knee replacement, may be required.
Early-stage AVN can often be managed without surgery, while advanced stages may necessitate more invasive treatments to restore joint function and reduce pain.
Non-Surgical Treatments for Avascular Necrosis
Not all cases of AVN require surgery. Early-stage AVN can be treated with non-invasive methods to reduce symptoms and slow the progression of the disease:
Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) help manage pain and reduce inflammation. Bisphosphonates may also be used to preserve bone density and slow damage.
Physical Therapy: A program focused on strengthening the muscles around the affected joint can help reduce stress on the bone and improve mobility.
Core Decompression: A minimally invasive procedure that involves drilling small holes into the bone to reduce pressure and increase blood flow, helping to prevent further damage.
Lifestyle Modifications: Resting the affected joint and avoiding high-impact activities can help prevent additional damage. Weight management and using assistive devices, like crutches, may also be recommended to ease pressure on the joint.
Recognizing the Symptoms of Avascular Necrosis
The symptoms of AVN usually develop gradually. The most common signs include:
Joint Pain: Often starting as mild discomfort, pain worsens over time, particularly with activity.
Stiffness: The affected joint may feel stiff, and range of motion can be limited.
Limping: If the hip or knee is affected, patients may start to limp to reduce pain.
Swelling: Some people experience swelling around the joint.
In the early stages, symptoms may be mild and go unnoticed. However, as the disease progresses, the pain becomes more intense and persistent.
Advances in Avascular Necrosis Treatment
Recent advancements have improved the treatment of avascular necrosis, offering new hope for patients:
Stem Cell Therapy: Stem cells may be used to regenerate bone tissue and stimulate blood flow, potentially reversing early-stage AVN.
Platelet-Rich Plasma (PRP): PRP injections, derived from the patient’s blood, can promote healing and reduce inflammation in the affected bone.
Minimally Invasive Techniques: Techniques like arthroscopy are being developed to treat AVN with smaller incisions, leading to faster recovery times and less trauma to the bone.
Biological Treatments: Researchers are investigating growth factors and other biological agents that can enhance bone healing and slow the disease’s progression.
These treatments are still in development, but they offer promising options for patients who might otherwise require invasive surgeries.
Recovery from Avascular Necrosis Treatment
Recovery after treatment depends on the severity of the condition and the type of treatment:
Non-Surgical Recovery: Patients who undergo non-invasive treatments, like physical therapy or medications, may start feeling relief within weeks, though it can take months for complete healing.
Post-Surgery Recovery: For those who undergo surgery, such as core decompression or joint replacement, recovery times can range from a few weeks for minimally invasive procedures to several months for joint replacement.
Physical Therapy: Rehabilitation is crucial for regaining joint function and mobility. Patients are typically advised to follow a customized exercise plan to rebuild strength.
Pain Management: Pain levels typically decrease as recovery progresses, but some patients may need long-term pain management strategies, especially in advanced stages.
Adhering to rehabilitation protocols and staying active within recommended limits can significantly improve long-term outcomes.
Diagnosing Avascular Necrosis: What You Need to Know
Diagnosing AVN early is crucial for effective treatment. The diagnosis typically involves:
X-rays: Initial imaging to identify bone changes or joint damage.
MRI (Magnetic Resonance Imaging): More sensitive and can detect early-stage AVN before bone collapse occurs.
CT Scan: Provides detailed images of the bone structure, often used in conjunction with MRI.
Bone Scans: Can identify changes in bone metabolism, revealing areas affected by AVN.
A doctor will also consider the patient’s medical history, symptoms, and risk factors to confirm the diagnosis and determine the stage of the condition.
Avascular Necrosis in Special Populations
Avascular necrosis affects people differently based on age, lifestyle, and underlying health conditions:
Young Patients: AVN is more challenging in younger patients, often requiring more aggressive treatments like joint replacement. They may also face long-term complications, such as needing multiple surgeries.
Athletes: AVN in athletes can result from repetitive trauma or steroid use. Early diagnosis and treatment are crucial to prevent long-term joint damage and career-ending injuries.
Patients with Chronic Diseases: Individuals with conditions like lupus, diabetes, or sickle cell anemia are at higher risk for AVN due to poor blood circulation. Managing these conditions is key to preventing or controlling AVN.
Pregnant Women: While rare, AVN can occur during pregnancy, especially in cases of corticosteroid use or other risk factors. Special care is required to balance treatment options with maternal health.
Treatment approaches for these groups often require customized care plans that consider their specific needs and risks.
Pain Management and Quality of Life with Avascular Necrosis
Pain is a central concern for patients with AVN, but there are several strategies to manage it:
Medications: NSAIDs and pain relievers are commonly used to manage mild to moderate pain. In more severe cases, stronger medications like opioids may be prescribed short-term.
Alternative Therapies: Techniques such as acupuncture, physical therapy, and aquatic exercises can help reduce pain and improve mobility without relying on drugs.
Surgical Relief: For those undergoing joint replacement, pain relief is often significant, and many patients report an improved quality of life post-surgery.
Long-Term Pain Management: Ongoing pain management strategies, such as low-impact exercise and weight control, can help maintain joint health and prevent further deterioration.
By managing pain effectively, patients can maintain a better quality of life and avoid debilitating effects.
Understanding the Cost of Avascular Necrosis Treatment
The cost of treating avascular necrosis can vary depending on the stage of the disease and the type of treatment required:
Non-Surgical Treatment: Medications, physical therapy, and core decompression are less expensive but may require ongoing care. Costs for these treatments can range from a few hundred to several thousand dollars.
Surgical Treatment: More complex procedures like bone grafting, osteotomy, or joint replacement surgery come with significantly higher costs. Joint replacement can range from $15,000 to $50,000 or more, depending on location and the type of surgery.
Insurance Coverage: Many health insurance plans cover the costs of surgery, medications, and rehabilitation, but coverage can vary. It's important to check with your insurance provider to understand what is covered.
Financial Assistance: Some hospitals offer financial aid or payment plans for patients in need. Additionally, government and nonprofit organizations may provide financial support for medical expenses.
Understanding the cost and exploring insurance options or financial aid can help reduce the financial burden of treatment.
Preventing Avascular Necrosis: Tips for Bone Health
While it may not be possible to fully prevent AVN, there are several steps people can take to reduce their risk:
Limit Steroid Use: Long-term use of corticosteroids is a major risk factor. If steroids are necessary, work with your doctor to manage doses and duration.
Moderate Alcohol Consumption: Excessive alcohol use can lead to bone damage and impaired blood flow. Limiting alcohol intake helps maintain bone health.
Healthy Diet: Eating a balanced diet rich in calcium, vitamin D, and other bone-supporting nutrients is essential for maintaining bone density.
Exercise: Regular, low-impact exercises like swimming or walking can help maintain joint health without putting excessive strain on the bones.
Early Detection: Regular check-ups and imaging studies for people with risk factors (e.g., those with a history of trauma or steroid use) can catch AVN early, improving the chances of successful treatment.
Maintaining overall bone health can reduce the likelihood of developing AVN or other bone-related conditions.
Global Trends in Avascular Necrosis Treatment
Treatment approaches for avascular necrosis vary around the world, reflecting differences in healthcare systems, technology, and medical practices:
Developed Countries: Advanced medical technologies like MRI, CT scans, and minimally invasive surgeries are more widely available. In countries like the U.S. and Europe, options like stem cell therapy and joint replacement are becoming more common.
Developing Countries: Access to high-quality healthcare may be limited, and many patients only receive treatment in the later stages of the disease. However, there is growing awareness of AVN, leading to improvements in diagnosis and treatment options in these regions.
Global Research: International collaborations and research are advancing the field of AVN treatment. Countries with high medical research output, such as Japan and South Korea, are at the forefront of innovative therapies like biological treatments and regenerative medicine.
The global trend is moving toward earlier diagnosis and more personalized, minimally invasive treatments. As awareness grows, more people worldwide have access to effective care.
How to Support a Loved One with Avascular Necrosis
Supporting someone with avascular necrosis involves both physical and emotional care:
Encourage Treatment: Help them stay on track with their treatment plan, whether it’s attending doctor’s appointments, taking medications, or following rehabilitation exercises.
Assist with Mobility: Offer help with daily activities, such as walking, getting in and out of chairs, and carrying items. Using assistive devices like crutches or a walker can improve mobility.
Provide Emotional Support: AVN can be a challenging condition to cope with, especially when pain and limited movement affect daily life. Listening and offering encouragement can significantly boost their morale.
Promote Self-Care: Help them engage in activities that they enjoy and can still participate in. This might include watching movies, doing light exercises, or simply spending quality time together.
Your support can have a big impact on their recovery process and emotional well-being.
Alternative and Complementary Therapies for Avascular Necrosis
In addition to conventional treatments, some patients seek alternative or complementary therapies to manage avascular necrosis:
Acupuncture: This traditional Chinese medicine technique involves inserting thin needles into specific points of the body to promote circulation and reduce pain.
Chiropractic Care: Some people with AVN turn to chiropractic adjustments to improve mobility and relieve pressure on affected joints, though this is more commonly used in combination with other treatments.
Herbal Remedies: Certain herbs, such as turmeric and ginger, are known for their anti-inflammatory properties and may be used to reduce pain and swelling associated with AVN.
Nutritional Supplements: Supplements like glucosamine, chondroitin, and omega-3 fatty acids are thought to support joint health and reduce inflammation. However, their effectiveness in treating AVN specifically requires more research.
While these therapies can provide symptom relief, they should be used in conjunction with conventional medical treatments under the guidance of a healthcare professional.
Future Outlook for Avascular Necrosis Treatment
The future of AVN treatment holds promise due to ongoing advancements:
Regenerative Medicine: Research into stem cell therapies, gene therapy, and tissue engineering may soon offer ways to regenerate damaged bone tissue and restore blood flow to the affected areas.
Personalized Treatments: With advances in genetics and technology, treatments tailored to an individual's specific needs may become more widespread, improving outcomes and reducing the risk of complications.
Improved Prosthetics: For patients requiring joint replacements, future prosthetics may offer better durability, more natural motion, and faster recovery times.
Early Detection Methods: New imaging technologies and biomarkers are being developed to detect AVN at earlier stages, allowing for quicker intervention and potentially preventing the need for invasive procedures.
Continued research and innovation are likely to lead to even more effective treatments in the coming years, improving outcomes for AVN patients globally.
Conclusion
Avascular necrosis is a challenging condition, but with early diagnosis and appropriate treatment, many individuals can manage their symptoms and improve their quality of life. Whether through non-surgical methods like medication and physical therapy, or more advanced options like joint replacement, there are effective treatments available.
As research continues to evolve, new therapies and technologies are paving the way for better outcomes. It’s crucial for patients to work closely with healthcare providers to determine the best approach for their specific needs. With proper care, individuals with AVN can lead active, fulfilling lives.