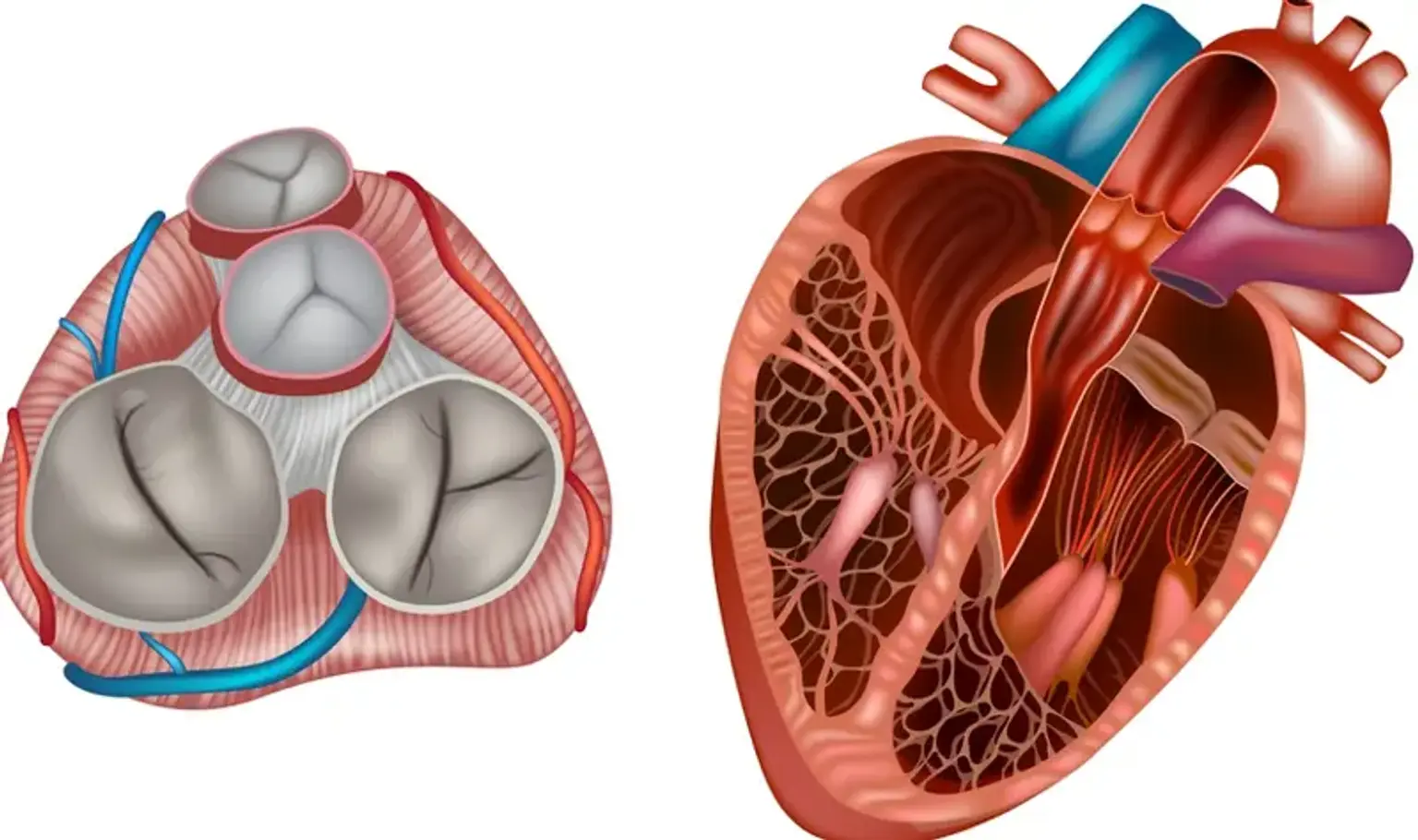
Organic Tricuspid Valve Repair
Overview
The tricuspid valve is one of four heart valves. It is situated between the right lower (right ventricle) and right upper (right atrium) cardiac chambers. The tricuspid valve opens and shuts to keep blood flowing in the right direction. The right atrioventricular valve is another name for it.
The heart circulates blood through four chambers in a certain order (two atria and two ventricles). The atria receive oxygen-depleted blood from the body every time your heart beats. In order to push blood out, the ventricles contract (squeeze). Valves open and shut when the heart beats, allowing blood to flow from one part of the heart to another. The valves aid in ensuring that blood flows at the proper time and in the proper direction.
Blood travels from the right atrium to the right ventricle via the tricuspid valve. It also stops blood from returning between those two chambers. The tricuspid valve opens as the right atrium fills, allowing blood to enter the right ventricle. The right ventricle then contracts, sending blood to the lungs. The tricuspid valve shuts firmly, preventing blood from flowing backward into the right atrium.
If the tricuspid valve isn't working properly, blood may not flow as effectively in the right direction or may leak in the incorrect way. It is possible that your heart will have to work harder to pump adequate blood to the rest of your body.
Tricuspid valve disorders are classified into three types:
- Tricuspid atresia: Tricuspid atresia is an inherited structural heart abnormality. In this case, the valve is replaced by a solid piece of tissue. This restricts blood flow and might result in right ventricular underdevelopment. Surgery is frequently required.
- Tricuspid regurgitation: This problem occurs when blood leaks backward via the tricuspid valve.
- Tricuspid stenosis: The tricuspid valve opening is excessively small in this disease, limiting blood flow between the two chambers.
What are tricuspid valve replacement and repair?
Tricuspid valve replacement and repair are procedures used to address illnesses of the tricuspid valve in your heart. The tricuspid valve is one of four valves in your heart that govern blood flow. It is located on the right side of your heart, between the upper (atrium) and lower chambers (ventricle). It ensures that blood flows from the right atrium to the right ventricle in the proper direction. As blood passes through the tricuspid valve, three flaps called leaflets open and close.
In general, healthcare specialists suggest utilizing your own heart tissue for healing whenever feasible. However, if the valve and surrounding tissue are severely damaged, your doctor may propose a replacement valve.
Replacement valves are classified into two types: biological and mechanical. A biological valve can be derived from either an animal or a deceased human donor. A mechanical valve is a medical gadget that has been produced. You may not need to take blood thinners after receiving a valve from an animal or human donor. However, because mechanical valves increase the danger of blood clots, you will need to take blood thinners for the rest of your life.
What conditions need tricuspid valve repair/replacement?
Tricuspid valve disorder refers to a group of medical diseases that impact the function of the tricuspid valve. The most common types are:
- Tricuspid regurgitation: The valve leaks or fails to seal properly, enabling blood to stream backward.
- Tricuspid stenosis: The leaflets of the valve are overly stiff, causing blood flow to be restricted.
When the tricuspid valve fails to function properly, your heart may have to work harder to provide blood to your body. This might result in uncomfortable symptoms and problems such as heart failure.
The most prevalent reason for tricuspid valve repair is tricuspid regurgitation (TR). In the United States, an estimated 1.6 million people have moderate to severe tricuspid regurgitation, with just a few thousand tricuspid valve repair surgeries performed each year. Over a ten-year period, 5005 primary tricuspid valve operations were conducted, with an 8.8% in-hospital death rate.
There is rising interest in the treatment of solitary tricuspid valve diseases due to solid evidence that untreated severe tricuspid regurgitation results in a deteriorated prognosis. Tricuspid regurgitation has been linked to an increased risk of cardiac events and death in people with congestive heart failure.
Despite the fact that tricuspid valve defects can cause severe morbidity and death, isolated tricuspid valve repair is uncommon. The majority of tricuspid valve surgeries are done in conjunction with other main cardiac surgical procedures. The most prevalent reason for tricuspid valve surgery nowadays is in individuals with symptomatic severe primary tricuspid regurgitation. The following conditions warrant tricuspid valve repair or replacement:
- Symptomatic severe tricuspid stenosis
- Severe tricuspid stenosis without symptoms while the patient is receiving left-sided valve surgery
- Severe primary or secondary tricuspid regurgitation with symptoms
- Severe primary or secondary tricuspid regurgitation (symptomatic or asymptomatic) during left-sided valve surgery
- Moderate to severe primary tricuspid regurgitation while the patient is undergoing valve surgery on the left side
- Primary tricuspid regurgitation that is asymptomatic or minimally symptomatic, with signs of growing right ventricular dilatation and dysfunction
- Mild to severe progressive functional (secondary) tricuspid regurgitation with a dilated annulus (more than 40 mm or greater than 21 mm/m2) while the patient is having left-sided valve surgery.
- Tricuspid valve endocarditis
- Carcinoid involvement of the tricuspid valve
- Congenital malformations e.g., Ebstein anomaly
- Traumatic or iatrogenic injuries to the valve when taking biopsies or from pacemaker leads
How is tricuspid valve repair done?
Preparation:
Your medical condition will be evaluated by your healthcare practitioner prior to tricuspid valve surgery. Your surgeon will examine your tricuspid valve using echocardiography and cardiac catheterization. These tests will also aid in the planning of your operation.
Echocardiography is a cardiac ultrasound that examines the valve and muscle function. Cardiac catheterization is a procedure that examines blood flow through the arteries of the heart muscle and measures pressures inside the heart and lungs.
- Your healthcare professional will go through the process with you. Discuss any concerns you have with your healthcare practitioner.
- You will sign a consent form granting authorization to do the surgery. If something is unclear, read the form carefully and ask questions.
- Before performing the treatment, your healthcare professional may do a comprehensive physical checkup to confirm you are in generally good health. You may be subjected to blood testing or other diagnostic procedures.
- Follow any instructions for not eating or drinking before surgery.
- You may be instructed to shower with an antibacterial scrub the night before or the morning before surgery to avoid infection of the incision areas.
- Inform your healthcare practitioner immediately if you are pregnant or suspect you may be pregnant.
- Tell your healthcare provider:
-
- If you are sensitive to or allergic to any medications, iodine, latex, tape, or anesthesia (local and general)
- About any prescription and over-the-counter medications, as well as herbal supplements, that you use. Certain medications may need to be discontinued prior to surgery. Follow your healthcare provider's advice regarding which medications should be discontinued and when.
- If you have a history of bleeding problems or are on any blood-thinning (anticoagulant) medications, aspirin, or other treatments that alter blood clotting. Some of these medications may be discontinued prior to the operation. Before the treatment, your healthcare professional may require a blood test to evaluate how long it takes your blood to clot.
- If you have a pacemaker or other cardiac device inserted.
- If you smoke, quit as soon as possible before to the treatment. This may increase your chances of a good surgical recovery and help your overall health.
Procedure:
A hospital stay is frequently required after heart valve repair surgery. Procedures may differ based on your illness and the methods of your surgeon. In general, heart valve repair surgery proceeds as follows:
- You will be instructed to remove any jewelry or other things that might obstruct the operation.
- An IV (intravenous) line will be placed in your arm or hand by a healthcare expert. Before the surgery, you may be given IV antibiotics.
- Other catheters may be implanted in your neck and wrist to monitor your heart and blood pressure, as well as to collect blood samples. Catheters can also be placed behind the collarbone and in the groin.
- During the procedure, the anesthesiologist will check your heart rate, blood pressure, respiration, and blood oxygen level. After you've been sedated, a breathing tube may be put through your throat into your lungs, and you'll be connected to a ventilator, which will breathe for you during the procedure.
- A nurse will insert a catheter into your bladder to drain urine.
- Your surgeon will implant a transesophageal echocardiography (TEE) probe into your esophagus to assess valve function following repair.
- An antiseptic solution will be applied to the skin over the surgical site by a member of the surgical team.
- From just below the Adam's apple to just above the navel, the surgeon will create an incision (cut) along the middle of the chest.
- Using a special surgical instrument, the doctor will cut the sternum (breastbone) in half lengthwise. To reveal the heart, the two parts of the breastbone will be removed and stretched apart.
- Your surgeon will need to halt the heart in order to accomplish this delicate valve surgery. Before the heart is stopped, tubes are implanted so that blood may be pumped through your body by a cardiopulmonary bypass machine.
- After diverting the blood to the heart-lung bypass machine for pumping, your surgeon will stop the heart by injecting it with a cold solution.
- Once the heart has stopped, the mending process will begin. The process employed will be determined by the type of valve problem you have, such as separation of fused valve leaflets, repair of torn leaflets, or reshaping of valve sections to improve performance.
- After the surgery, your surgeon will enable the blood moving via the bypass machine to re-enter your heart. To restart your heart's electrical activity, they will shock it with little paddles. Your heart will gradually begin pumping blood across your body. The tubes that link you to the heart-lung machine will be removed by your surgeon.
- Once your heart is beating again, the surgeon will check the function of the heart and the valves.
- Your surgeon may put temporary pacing wires into your heart. These wires can be connected to a pacemaker and, if necessary, your heart can be paced throughout the early recovery phase.
- Your surgeon may place tubes in your chest to remove blood and other fluids from the area surrounding your heart. To drain fluids away from the heart, these tubes will be attached to a suction device.
- Your surgeon will reconstruct the sternum.
- Your surgeon will reattach the skin above the sternum and seal it with stitches or staples.
- A tube may be inserted through your mouth or nose into your stomach to drain stomach fluids.
- A sterile bandage or dressing will be applied.
If your surgeon performs a minimally invasive treatment, special tools will be inserted into your chest through numerous minor incisions rather than a single big incision. These tools will include a camera as well as all of the equipment required to fix your valve. Although this operation may take longer than typical open-heart surgery, recovery may be simpler.
Minimally invasive tricuspid valve replacement often entails no incisions (if performed via catheter) or fewer incisions, as well as a shorter hospital stay than standard open-heart surgery. Balloon valvuloplasty (also known as balloon valvuloplasty or balloon valvotomy) is a minimally invasive technique that is frequently used to treat babies and children with tricuspid valve stenosis.
A surgeon inserts a thin, hollow tube (catheter) into a blood artery, usually in the groin, and threads it to the heart during balloon valvuloplasty. A balloon at the catheter's tip is inflated, widening the restricted tricuspid valve. The balloon is deflated and taken away.
Catheter-based methods are being developed to address tricuspid valve regurgitation in some individuals who are not surgical candidates. In exceptional instances, a health care practitioner may explore this possibility with you.
How is organic tricuspid valve replacement done?
If the tricuspid valve cannot be repaired, surgery to replace the valve may be required. Tricuspid valve replacement surgery can be performed either open-heart or minimally invasively. A surgeon removes the damaged or diseased valve and replaces it with a mechanical valve or a valve manufactured from cow, pig, or human heart tissue during tricuspid valve replacement (organic or biological tissue valve).
You and your healthcare experts will review the risks and advantages of each kind of valve to determine which one is best for you. Biological tissue valves do not necessitate the use of blood thinners for the rest of one's life. Tissue valves, on the other hand, can wear out over time and may need to be replaced.
If your biological tissue tricuspid valve has failed, a less invasive catheter treatment may be used instead of open-heart surgery to replace it. Using X-rays as a guide, the heart doctor (cardiologist) inserts a thin, hollow tube (catheter) into a vein and directs it to the tricuspid valve. Once in position, a replacement valve is inserted into the existing biological valve through the catheter. A valve-in-valve method is used to replace the tricuspid valve.
What happens after organic tricuspid valve repair/replacement?
You will usually be hospitalized for several days following tricuspid valve repair or replacement surgery. The length of your stay is determined on your health and the type of tricuspid valve surgery you get.
During the hospital stay, you may have:
- An IV to receive fluids and medications
- Tubes to drain urine from your bladder
- Tubes to drain fluid and blood from your heart and chest
Your care providers will:
- Check for infection at your incision sites
- Regularly check your blood pressure, breathing and heart rate
- Help you manage pain after surgery
- Ask you to take longer and longer walks to increase your activity
- Show you how to do breathing exercises as you recover
Following tricuspid valve repair or replacement surgery, your health care team will provide you instructions to follow. These instructions usually include information regarding the following:
- The medications you've been prescribed
- The warning signs and symptoms of infection
- How to care for your incisions
- How to manage pain
- Side effects of surgery
What are the possible complications following tricuspid valve repair/replacement?
Every procedure has some level of risk. The risks of tricuspid valve repair and replacement vary depending on the treatment, your overall health, and the doctors' skill. Consider having your tricuspid valve repaired or replaced at a medical center that has a multidisciplinary team of heart surgeons and care providers who are trained and skilled in heart valve surgery.
The following risks are connected with tricuspid valve repair and replacement surgery:
- Bleeding
- Blood clots
- Failure of a replacement valve
- Irregular heart rhythms (arrhythmias)
- Infection
- Stroke
- Death
To avoid an infection (endocarditis) around the new heart valve or ring, you should be given antibiotics before any surgery that might let germs into your body. These procedures are as follows:
- All dental procedures (cleaning, filling, removing teeth, root canal, gum or ulcer treatment).
- Surgical procedures such as colonoscopy and cystoscopy.
The valve manufacturer will provide you with an identity card including information on the kind and size of your heart valve. Keep it with you at all times. Remember to inform any doctor or dentist who is treating you about your valve and the requirement for antibiotics.
Organic vs mechanical tricuspid valve
The valve used for tricuspid replacement is debatable. Initially, mechanical prostheses were used, but in most cases, bioprosthetic valves have taken their place. In reality, the bioprosthesis is more durable in the right heart due to lower pressure and stress than in the left heart.
In contrast to mechanical valves, which have a higher risk of thrombosis and bleeding, bioprosthetic valves do not require long-term anticoagulation. Mechanical valves, on the other hand, have advantageous hemodynamic qualities, such as low gradients, low flow disruptions, and extended durability.
The average lifespan of a tricuspid bioprosthesis is 7 years. Bioprostheses are favored because they do not require anticoagulation while also having a longer durability and a lower reoperation rate when compared to alternative left sided heart valve locations. They are also preferable when anticoagulation is contraindicated, such as during pregnancy or in older age groups with a short life expectancy.
Mechanical valves, on the other hand, are favored in younger age groups and in patients who have another mechanical valve in place. After one year, the overall independence from thromboembolism problems was 92.6%. The majority of studies found no significant differences in hemodynamic parameters or early and late problems between bioprosthetic and mechanical valves.
Conclusion
Tricuspid valve replacement and repair are surgical techniques used to treat one of the four heart valves. If you have tricuspid regurgitation or stenosis, consult your cardiologist to see if this type of surgery will assist.
The tricuspid repair is the first option for tricuspid surgery; however, due to significant structural valve malfunction, the valve must occasionally be replaced. Tricuspid valve surgery accounts for 5.7% of all valvular operations, whereas tricuspid valve replacement accounts for 1.7% of all tricuspid valve surgeries.
Patients who have had mitral and/or aortic valve surgery in addition to tricuspid valve surgery have a high-risk operation and a bad prognosis. The second and last option in tricuspid valve surgery is tricuspid valve replacement. The decision between inserting a mechanical or bioprosthetic valve remains debatable.
Patients who require tricuspid valve replacement are often high-risk surgical candidates with a high risk of both early and late death. Right ventricular failure was the leading cause of mortality. However, the decision between mechanical and biological valves remains debatable.
Report any symptoms that might indicate a problem with the valve or the heart after tricuspid valve surgery:
- Dizziness or lightheadedness.
- Extreme fatigue.
- Sudden weight gain.
- Swelling in your feet or ankles.
Call your doctor if you experience any of the following symptoms of infection:
- Chills.
- Draining or oozing from the incision.
- Fever.
- Pain that gets worse.
- Redness around the incision site.
Seek emergency medical attention if you have any of the following symptoms, which might signal a life-threatening issue with heart function:
- Chest pain.
- Pressure or tightness in your chest.
- Sudden severe shortness of breath.
- Fainting.